Understanding Thyroid Diseases: Symptoms, Diagnosis, and Treatment Options
Thyroid health is often overlooked, yet it plays a pivotal role in regulating metabolism, energy levels, and overall well‑being. Whether you’re experiencing unexplained fatigue, sudden weight changes, or subtle mood swings, thyroid disorders could be the underlying cause. This comprehensive guide breaks down the anatomy of the thyroid, explores common conditions such as hypothyroidism and hyperthyroidism, and outlines modern diagnostic and treatment strategies.
1. Anatomy and Function of the Thyroid Gland
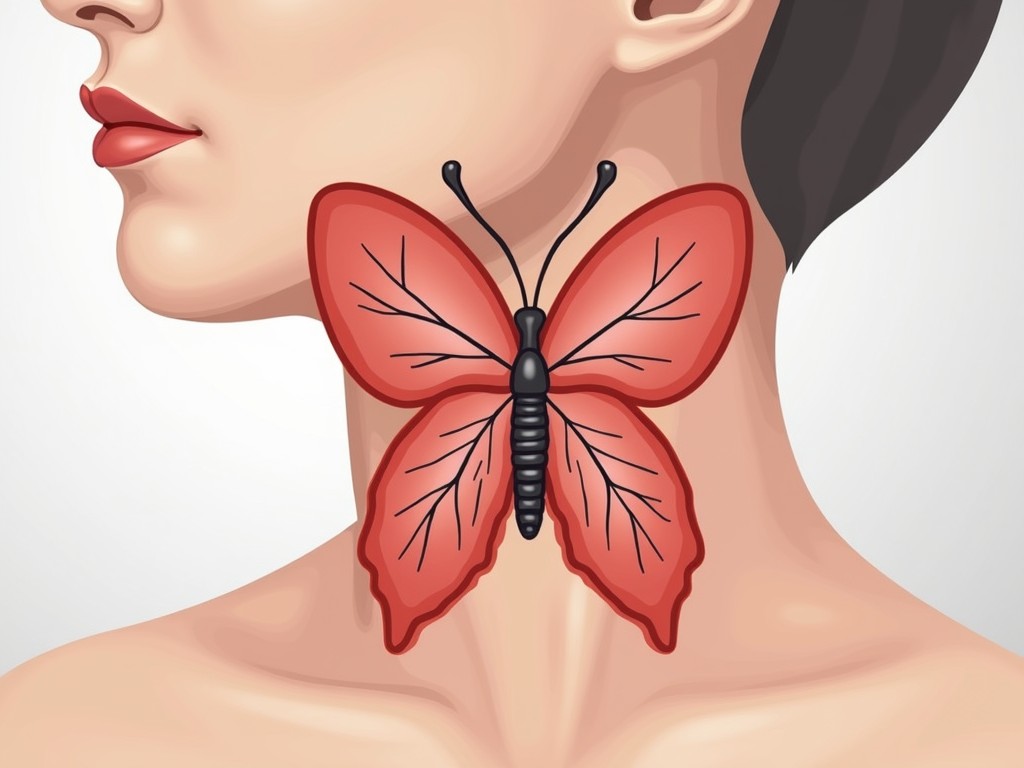
The thyroid is a butterfly‑shaped gland located in the front of the neck, just below the Adam’s apple. Weighing roughly 15–20 grams, it produces two key hormones: triiodothyronine (T3) and thyroxine (T4). These hormones control the body’s metabolic rate, influencing everything from heart rate to body temperature and even brain function.
Key Functions
- Regulates metabolism and energy production
- Influences body temperature and oxygen consumption
- Supports brain development and cognitive function
- Modulates carbohydrate metabolism and lipid profiles
2. Common Thyroid Disorders
Thyroid diseases can be broadly categorized into functional and structural abnormalities. Below we detail the most prevalent conditions.
2.1 Functional Disorders
Hypothyroidism
When the thyroid produces insufficient hormones, the body’s metabolic processes slow down. Symptoms may include:
- Persistent fatigue and low energy
- Weight gain or difficulty losing weight
- Cold intolerance and feeling cold all the time
- Dry, pale skin and hair loss
- Constipation and muscle cramps
- Depression or memory problems
Hashimoto’s thyroiditis—an autoimmune attack on thyroid tissue—is the leading cause of hypothyroidism, especially in women. Other triggers include iodine deficiency, certain medications, and radiation exposure.
Hyperthyroidism
Excessive hormone production accelerates metabolism, leading to:
- Unexplained weight loss
- Rapid heartbeat or palpitations
- Heat intolerance and excessive sweating
- Hand tremors and anxiety
- Bulging eyes (Graves’ disease)
- Increased appetite
Graves’ disease, toxic nodular goiter, and thyroiditis are common causes. Over‑supplementation with iodine or certain medications can also trigger hyperthyroidism.
2.2 Structural Disorders
Goiter
A goiter is an enlargement of the thyroid gland. It can be:
- Diffuse—uniform swelling
- Nodular—one or more distinct lumps
While many goiters are benign, they may compress the trachea or esophagus, causing breathing or swallowing difficulties.
Thyroid Nodules
These are localized clusters of thyroid cells that can be:
- Hot (functioning)—producing excess hormones
- Cold (non‑functioning)—often benign but may harbor cancer
Ultrasound and fine‑needle aspiration biopsy are the gold standards for evaluating nodules.
Thyroiditis
Inflammation of the thyroid can cause transient hyperthyroidism followed by hypothyroidism. Common types include Hashimoto’s, subacute (de Quervain’s), and postpartum thyroiditis.
Thyroid Cancer
Although rare, thyroid cancer is the most common endocrine malignancy. The main subtypes are:
- Papillary (most common, excellent prognosis)
- Follicular (more likely to spread to distant organs)
- Medullary (associated with genetic syndromes)
- Anaplastic (aggressive, rare)
Risk factors include high radiation exposure, family history, and certain genetic syndromes.
3. Diagnosis: How Doctors Identify Thyroid Issues
Accurate diagnosis relies on a combination of clinical evaluation and laboratory tests:
- TSH (Thyroid Stimulating Hormone)—primary screening test; high in hypothyroidism, low in hyperthyroidism.
- T4 and T3 levels—confirm hormone status.
- Ultrasound—visualizes nodules, goiter size, and vascularity.
- Radioactive iodine uptake—assesses functional activity of nodules.
- Fine‑needle aspiration biopsy—diagnoses malignancy.
4. Treatment Options
4.1 Hypothyroidism
Standard therapy is levothyroxine replacement. Key points:
- Start with a low dose and titrate based on TSH levels.
- Monitor every 6–12 months after stabilization.
- Adjust dose during pregnancy, menopause, or significant weight changes.
4.2 Hyperthyroidism
Treatment depends on severity and underlying cause:
- Antithyroid drugs (methimazole, propylthiouracil) to block hormone synthesis.
- Radioactive iodine therapy to ablate overactive tissue.
- Beta‑blockers for symptom control (palpitations, tremor).
- Surgery (partial or total thyroidectomy) for large goiters or suspicious nodules.
4.3 Nodules and Goiter
Management ranges from observation to surgical removal:
- Small, asymptomatic nodules: periodic ultrasound surveillance.
- Large or symptomatic nodules: surgical excision or radioactive iodine.
- Biopsy‑confirmed malignancy: total thyroidectomy ± neck dissection.
4.4 Thyroid Cancer
Primary treatment is surgical removal of the thyroid (total or lobectomy). Post‑operative care may include:
- Levothyroxine suppression therapy to inhibit TSH.
- Radioactive iodine ablation for residual tissue or metastatic disease.
- Regular follow‑up with ultrasound and thyroglobulin levels.
5. Frequently Asked Questions
Q: Can I get thyroid disease from a normal diet?
A: While iodine deficiency is a common cause, most thyroid disorders arise from autoimmune processes or genetic predispositions. A balanced diet with adequate iodine usually suffices.
Q: Are thyroid tests necessary for everyone?
A: Routine screening is recommended for high‑risk groups—women over 60, those with a family history, or individuals with autoimmune diseases. Otherwise, testing is symptom‑driven.
Q: Will thyroid medication affect my pregnancy?
A: Levothyroxine is safe and essential during pregnancy to prevent fetal hypothyroidism. Dosage adjustments are often required.
6. Conclusion
Thyroid disorders, though common, are highly treatable when identified early. Understanding the gland’s role, recognizing symptoms, and pursuing appropriate diagnostics can dramatically improve quality of life. If you suspect thyroid issues—especially if you’re experiencing unexplained fatigue, weight changes, or mood swings—consult a healthcare professional for evaluation. With timely intervention, most patients achieve normal metabolic function and return to their daily activities with renewed vigor.