Ulnar Nerve Injury: Symptoms, Diagnosis, and Effective Treatment Options
Introduction
Have you ever felt a sudden numbness in your little finger or struggled to grip a pen? These seemingly minor issues can be early warning signs of an ulnar nerve injury. The ulnar nerve, running from the shoulder down to the hand, plays a crucial role in sensation and motor control of the fingers. When it becomes compressed or damaged, everyday tasks can become frustrating and painful. This guide dives deep into the causes, symptoms, diagnostic methods, and treatment strategies for ulnar nerve injury, helping you recognize the problem early and take decisive action.
What Is an Ulnar Nerve Injury?
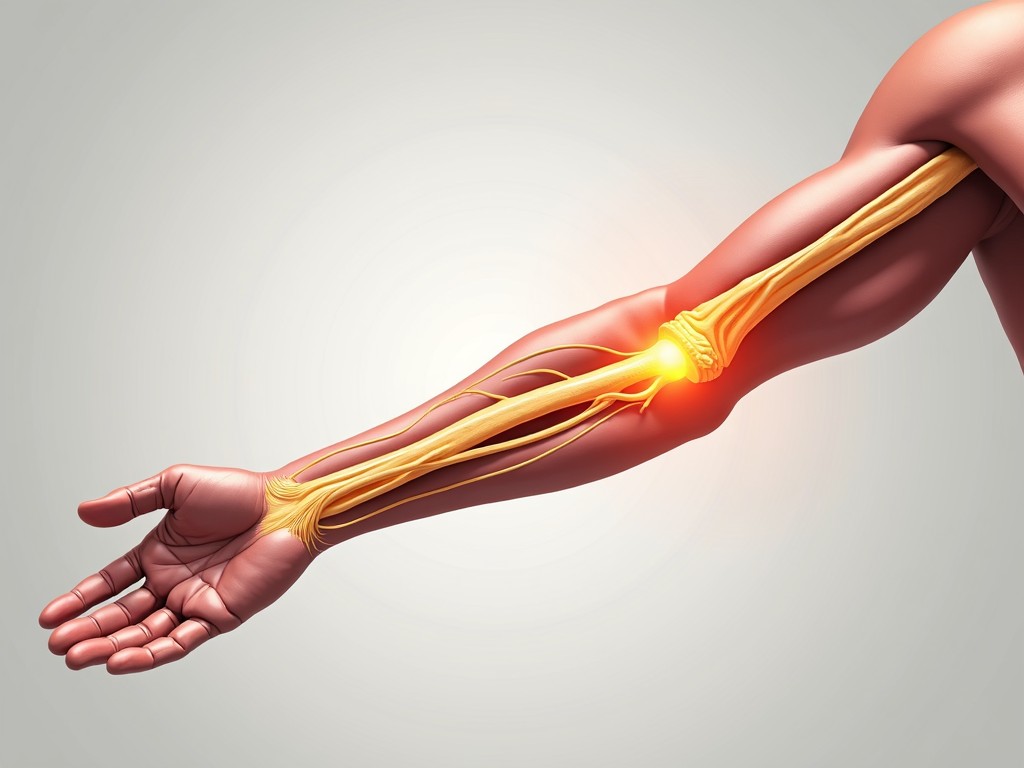
An ulnar nerve injury occurs when the nerve is damaged or compressed along its course from the shoulder, through the elbow, and into the hand. The nerve supplies sensation to the little and ring fingers and controls many intrinsic hand muscles. Damage can manifest as numbness, tingling, weakness, or even muscle wasting.
Common Causes
- Repetitive wrist or elbow movements (e.g., typing, playing sports)
- Traumatic injuries such as fractures or dislocations
- Prolonged pressure from a cast or splint
- Medical conditions like diabetes or thyroid disorders that affect nerve health
Types of Ulnar Nerve Injury
Ulnar nerve injuries are generally classified into two categories: benign (non‑malignant) lesions and malignant (severe) lesions. Understanding the distinction helps determine the urgency and type of treatment required.
Benign Ulnar Nerve Lesions
- Often caused by mild compression or minor trauma.
- Symptoms are usually reversible with early intervention.
- Common in office workers and athletes who use repetitive motions.
Malignant Ulnar Nerve Lesions
- Result from significant nerve damage or prolonged pressure.
- Can lead to permanent muscle atrophy and loss of hand function.
- Requires prompt medical evaluation and possibly surgical intervention.
Recognizing the Symptoms
Early detection is key. Below are the hallmark signs of ulnar nerve injury, divided by severity.
Benign Symptoms
- Light tingling or numbness in the little and ring fingers.
- Minor weakness in hand muscles.
- Occasional “pinched” feeling at the elbow or wrist.
- Pain that worsens with movement.
Severe Symptoms
- Intense numbness or tingling in the fingers.
- Noticeable muscle weakness or wasting.
- Difficulty gripping objects or performing fine motor tasks.
- Constant pain that interferes with daily activities.
Diagnosing Ulnar Nerve Injury
Accurate diagnosis involves a combination of clinical evaluation and diagnostic tests.
Clinical Examination
- Assessment of sensation in the little and ring fingers.
- Testing hand muscle strength and coordination.
- Checking for pain or tingling along the nerve pathway.
Electrodiagnostic Tests
- EMG (Electromyography) – measures electrical activity in muscles.
- Nerve Conduction Velocity (NCV) – evaluates how quickly signals travel along the nerve.
Imaging Studies
- Magnetic Resonance Imaging (MRI) – visualizes soft tissue and nerve compression.
- Ultrasound – useful for dynamic assessment of nerve movement.
Treatment Options
Treatment depends on the severity and duration of the injury. Options range from conservative measures to surgical procedures.
Conservative Management
- Rest and activity modification to reduce nerve irritation.
- Use of a splint or brace to immobilize the elbow or wrist.
- Physical therapy focusing on stretching and strengthening exercises.
- Non‑steroidal anti‑inflammatory drugs (NSAIDs) for pain relief.
When Surgery Is Needed
- Persistent symptoms despite conservative care.
- Evidence of severe nerve compression or damage on imaging.
- Loss of hand function or significant muscle atrophy.
- Common procedures include ulnar nerve decompression or transposition to relieve pressure.
Recovery and Rehabilitation
Recovery timelines vary. Mild cases may improve within weeks, while surgical cases can require months of rehabilitation.
Post‑Treatment Care
- Regular physiotherapy sessions to rebuild strength and flexibility.
- Gradual reintroduction of activities to avoid re‑injury.
- Monitoring for signs of recurrence or new symptoms.
Frequently Asked Questions
Can ulnar nerve compression be prevented?
Yes. Ergonomic adjustments, regular breaks during repetitive tasks, and strengthening exercises can reduce the risk.
Will I recover fully if I have a severe ulnar nerve injury?
Recovery depends on the extent of damage and how quickly treatment begins. Early intervention often leads to better outcomes.
Is surgery always required for ulnar nerve injury?
No. Many cases respond well to conservative measures. Surgery is reserved for persistent or severe cases.
Conclusion
Ulnar nerve injury may start with subtle symptoms but can quickly progress to debilitating hand dysfunction if left untreated. By recognizing early signs—such as tingling in the little finger or mild hand weakness—and seeking prompt medical evaluation, you can prevent permanent damage. Whether managed conservatively or surgically, a tailored treatment plan combined with diligent rehabilitation offers the best chance for full recovery and a return to normal daily activities.