Understanding Spinal Canal Stenosis: Causes, Symptoms, Diagnosis, and Modern Treatment Options
Spinal canal stenosis—commonly referred to as lumbar spinal stenosis when it affects the lower back—poses a significant health challenge for millions worldwide. As the spinal canal narrows, the spinal cord and nerve roots become compressed, leading to pain, numbness, and functional limitations. This article delves into the anatomy, risk factors, clinical presentation, diagnostic strategies, and the latest surgical and non‑surgical interventions that can restore mobility and improve quality of life.
What Is Spinal Canal Stenosis?
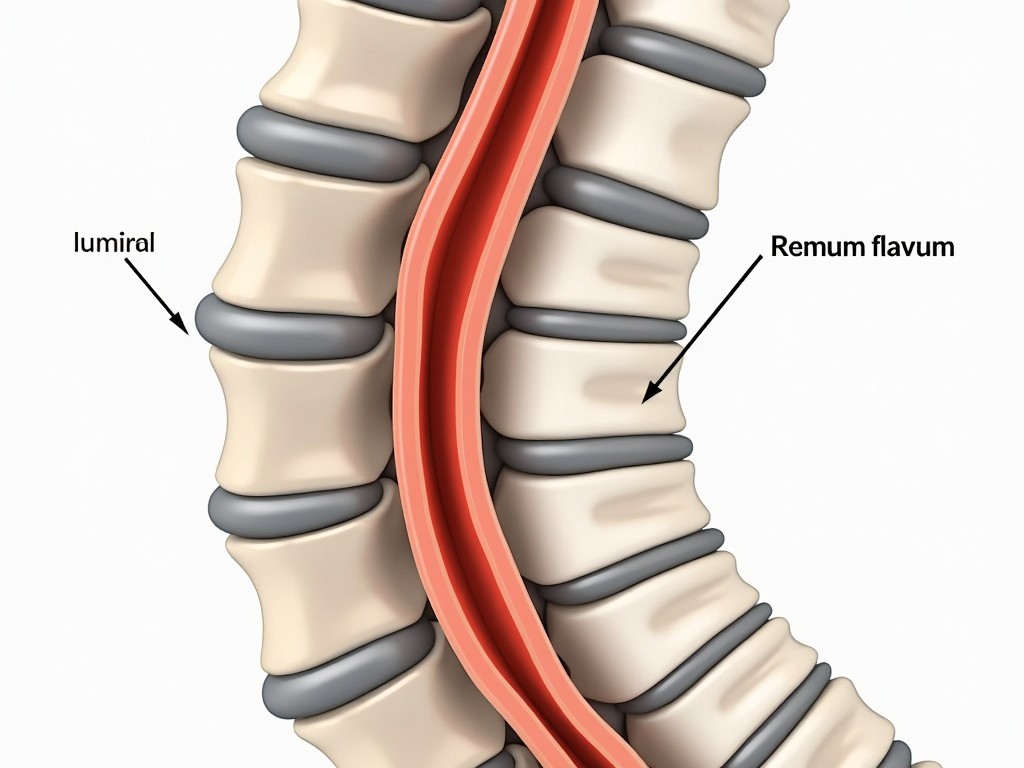
Spinal canal stenosis is the medical term for a narrowing of the spinal canal, the passageway that houses the spinal cord and nerve roots. The condition typically results from age‑related degeneration of the vertebrae, intervertebral discs, ligaments, and facet joints. Over time, these structures can ossify or thicken, encroaching on the canal space and exerting pressure on neural tissues.
Key Anatomical Players
- Ligamentum flavum – A yellow ligament that surrounds the spinal cord; it can calcify and thicken with age, contributing to canal narrowing.
- Facet joints – Small joints at the back of the spine that can develop osteophytes (bone spurs) that impinge on the canal.
- Intervertebral discs – Degeneration or herniation can push into the canal space.
- Vertebral bodies – Osteoporosis or vertebral fractures can alter the canal dimensions.
Who Is Most Affected?
While spinal stenosis can occur at any age, it is most common in individuals over 55. Women are slightly more prone than men, and those with a congenital narrow canal may experience symptoms earlier. Genetic predisposition, occupational hazards, and a history of spinal trauma also elevate risk.
Recognizing the Symptoms
Early signs often mimic other back problems, but certain features are characteristic:
- Neck or back pain that worsens with walking or standing and improves with bending forward or sitting.
- Radiating pain, tingling, or numbness in the arms (cervical stenosis) or legs (lumbar stenosis).
- Muscle weakness leading to difficulty walking or maintaining balance.
- Nighttime symptoms that awaken patients, often described as a “leg‑as‑a‑stick” feeling.
- In advanced stages, urinary incontinence, sexual dysfunction, or even paralysis may occur.
Diagnostic Pathways
Accurate diagnosis is critical for effective treatment. The typical work‑up includes:
- Clinical examination – Assessing gait, reflexes, and sensory deficits.
- Imaging – MRI provides detailed soft‑tissue contrast; CT scans are useful for bony detail. X‑rays can reveal alignment and degenerative changes.
- Electrodiagnostic studies – EMG and nerve conduction tests help differentiate stenosis from peripheral neuropathies.
Non‑Surgical Management: First‑Line Approach
When symptoms are mild to moderate, conservative care can be highly effective:
- Physical therapy – Strengthening core muscles, improving flexibility, and reducing load on the spine.
- Swimming and aquatic therapy – Low‑impact exercise that promotes circulation without stressing the joints.
- Medications – NSAIDs for pain and inflammation; muscle relaxants for spasms.
- Injections – Epidural steroid injections can provide temporary relief.
- Lifestyle modifications – Weight management, ergonomic adjustments, and avoiding prolonged standing or walking.
When Surgery Becomes Necessary
Progressive symptoms—such as frequent need for rest while walking, nighttime numbness that disrupts sleep, or loss of bladder control—signal the need for surgical intervention. Modern spine surgery offers several options, each tailored to the patient’s anatomy and overall health.
Traditional Decompression Techniques
Historically, surgeons performed laminectomies—removing the posterior vertebral arch—to widen the canal. While effective, this approach sometimes led to postoperative instability, especially when large portions of bone were removed.
Minimally Invasive Micro‑Decompression
Using high‑speed drills and microscopes, surgeons can precisely excise osteophytes and thickened ligaments through small incisions. Benefits include:
- Reduced blood loss and postoperative pain.
- Shorter hospital stays—many patients walk the same day.
- Lower risk of infection and faster return to daily activities.
Titanium Rod and Screw Stabilization
In cases where the spinal column is unstable—due to osteoporosis, fractures, or extensive bone removal—internal fixation with titanium rods and screws is employed. This technique restores alignment and prevents future collapse.
Three Golden Rules for Successful Outcomes
- Accurate Diagnosis – Ensuring the correct level and severity of stenosis.
- Experienced Surgeon – A specialist with a track record in spinal procedures.
- Optimal Hospital Environment – State‑of‑the‑art facilities and postoperative care teams.
Post‑Operative Recovery and Rehabilitation
After decompression, the body begins a gradual healing process. Key steps include:
- Early mobilization—walking with support as soon as possible.
- Rehabilitation exercises—targeting core stability and flexibility.
- Regular follow‑up imaging—to monitor fusion and hardware integrity.
- Patient education—on posture, ergonomics, and activity modification.
Frequently Asked Questions
Is spinal stenosis always caused by aging?
No. While degeneration is common, congenital narrowing, trauma, or inflammatory conditions can also lead to stenosis.
Can I avoid surgery entirely?
Many patients achieve significant relief with conservative measures, especially in early stages. Surgery is reserved for progressive or severe cases.
What is the success rate of minimally invasive decompression?
Studies report symptom improvement in 70–90% of patients, with low complication rates.
Conclusion
Spinal canal stenosis is a complex condition that demands a nuanced approach. Early recognition, precise diagnosis, and individualized treatment—whether conservative or surgical—are essential for preserving function and preventing irreversible damage. If you experience persistent back or leg pain, numbness, or nighttime symptoms, consult a spine specialist promptly. With the right care, you can regain mobility and return to the activities you love.