Eye Loss and Ocular Prosthesis: Comprehensive Guide to Rehabilitation and Recovery
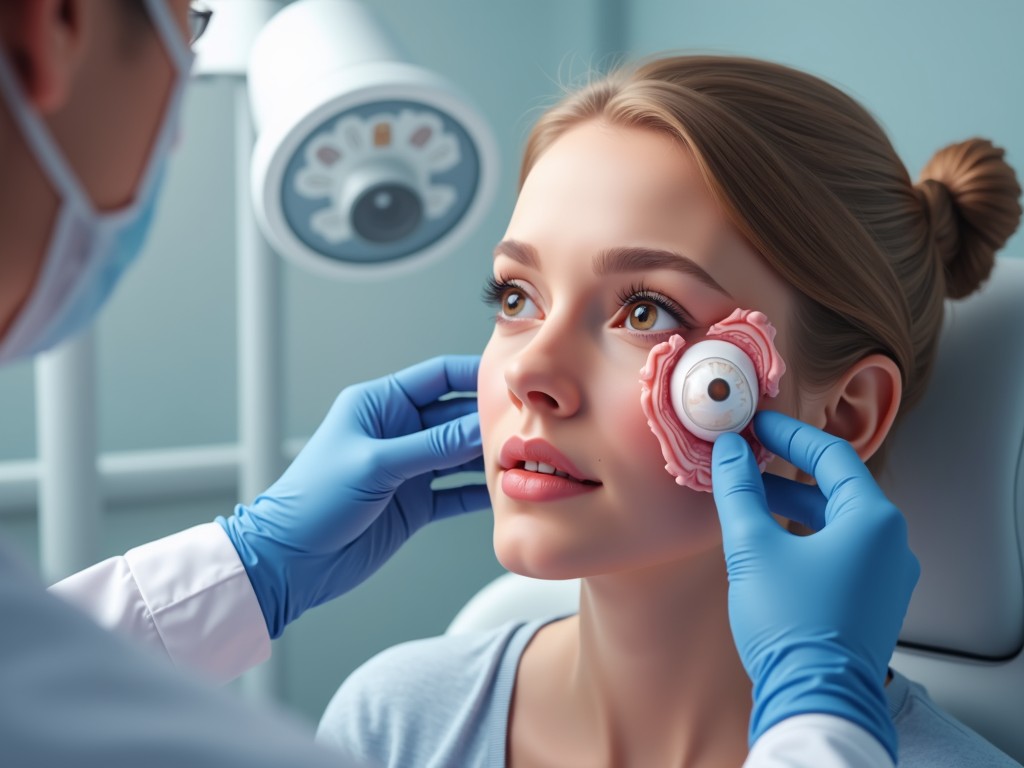
Eye loss—whether due to trauma, disease, or congenital absence—remains one of the most dramatic organ losses a person can experience. The psychological and functional impact is profound, yet the field of ocular prosthesis and eye rehabilitation offers powerful solutions that restore both appearance and confidence. This guide explores causes, treatment options, and the latest advances in prosthetic eye care.
Understanding the Causes of Eye Loss
Eye loss can arise from a variety of factors, each requiring a tailored approach:
- Trauma and Accidents – Blunt or penetrating injuries can damage the globe or surrounding structures.
- Infections and Inflammatory Diseases – Severe infections such as panophthalmitis or autoimmune conditions may necessitate removal.
- Eye Cancer – Basal cell carcinoma and other malignant tumors of the eyelid or orbit often require surgical excision.
- Congenital Anomalies – Some infants are born with microphthalmia (small eye) or anophthalmia (absent eye).
- Complications of Eye Surgery – Rarely, procedures like cataract extraction can lead to globe loss.
The Psychological Impact of Eye Loss
Beyond the physical loss, the absence of an eye can alter self‑image and social interactions. Studies show that patients who receive ocular prostheses report significant improvements in self‑esteem and social functioning. Early intervention—especially in children—helps prevent facial asymmetry and supports normal psychological development.
Rehabilitation Pathways: From Surgery to Prosthesis
1. Pre‑Prosthetic Surgical Planning
Before a prosthesis can be fitted, the eye socket (orbital cavity) must be prepared:
- Orbital Implants – Biocompatible materials (e.g., porous polyethylene) are placed to maintain volume and stimulate bone growth.
- Soft Tissue Reconstruction – Flap techniques restore eyelid function and protect the socket.
- Early Intervention in Children – Using spacers or temporary implants during growth phases prevents asymmetry.
2. Fabrication of the Ocular Prosthesis
Once the socket is ready, a custom prosthetic eye is crafted:
- Impression Taking – A precise mold of the socket ensures a snug fit.
- Color Matching – The prosthesis is tinted to match the patient’s natural iris and sclera.
- Attachment Mechanisms – Options include adhesive, magnetic, or implant‑anchored systems.
3. Post‑Fitting Care and Follow‑Up
Long‑term success depends on diligent care:
- Regular cleaning with mild soap and water.
- Routine check‑ups to assess socket health and prosthesis fit.
- Prompt reporting of discomfort, redness, or discharge.
Special Considerations for Different Patient Groups
Children with Congenital Eye Absence
Early intervention is critical. Pediatric teams often use:
- Temporary spacers to guide orbital growth.
- Delayed definitive prosthesis until the child is old enough for a custom fit.
- Multidisciplinary care involving ophthalmologists, plastic surgeons, and psychologists.
Adults with Trauma or Cancer‑Related Loss
In these cases, the focus is on:
- Rapid reconstruction to minimize scarring.
- Use of implantable prostheses for better stability.
- Psychological counseling to address body image concerns.
Common Questions About Eye Prostheses
What is the lifespan of an ocular prosthesis?
With proper care, a prosthesis can last 5–10 years. Replacement is often needed due to wear, changes in socket shape, or cosmetic updates.
Can I perform daily activities with a prosthetic eye?
Yes. Most patients resume normal activities, including driving and sports, once the prosthesis is comfortable.
Is the procedure painful?
During surgery, anesthesia ensures no pain. Post‑operative discomfort is usually mild and manageable with prescribed medications.
Emerging Trends in Ocular Prosthetics
Innovation is driving better outcomes:
- 3‑D Printing – Enables highly accurate, patient‑specific prostheses.
- Smart Materials – Incorporating sensors for ocular health monitoring.
- Regenerative Medicine – Research into tissue‑engineered eyelids and orbital implants.
Conclusion
Eye loss is undeniably challenging, but advances in ocular prosthesis technology and comprehensive rehabilitation strategies provide hope and tangible solutions. Early assessment, meticulous surgical preparation, and personalized prosthetic design are the pillars of successful recovery. Whether you are a patient, caregiver, or healthcare professional, understanding these steps can empower you to navigate the journey toward restored confidence and facial harmony.