Scar Treatment 2025: Comprehensive Guide to Healing, Prevention, and Cosmetic Solutions
Scar treatment is a topic that touches many lives, whether you’re recovering from a surgical incision, a burn, or an accidental cut. While scars are a natural part of the healing process, their appearance can affect confidence and comfort. This guide dives deep into the science of scar formation, evidence‑based treatments, and practical steps you can take to promote smoother, less noticeable scars. Whether you’re a patient, a caregiver, or a medical professional, the information below will help you navigate the journey from wound to healed skin.
Understanding How Scars Form
When the skin’s integrity is disrupted—by trauma, surgery, burns, or infection—your body initiates a complex repair process. The key stages are:
- Inflammation: Blood vessels dilate, bringing immune cells to the site.
- Proliferation: Fibroblasts produce collagen and new blood vessels.
- Remodeling: Collagen reorganizes over 1–2 years, gradually softening the scar.
Even after the scar has matured, subtle changes in color, texture, and thickness can persist. Factors such as wound depth, location, and individual genetics influence the final outcome.
Common Causes of Scarring
- Accidental cuts or lacerations
- Surgical incisions (e.g., breast augmentation, abdominoplasty)
- Burns and thermal injuries
- Infections and abscesses
- Acne, chickenpox, and other dermatologic conditions
- Traumatic injuries (car accidents, gunshot wounds)
Key Factors That Influence Scar Quality
Wound Characteristics
- Depth: Deeper wounds tend to produce thicker scars.
- Location: Areas with high tension (e.g., shoulders, chest) often scar more prominently.
- Orientation: Aligning incisions parallel to natural skin lines can reduce visibility.
Healing Environment
- Proper wound cleaning and dressing reduce infection risk.
- Maintaining adequate blood flow is essential; smoking impairs circulation.
- Sun protection prevents hyperpigmentation and accelerates remodeling.
Patient‑Related Factors
- Age: Younger skin heals faster but may produce more pronounced scars.
- Genetics: Some individuals are predisposed to keloids or hypertrophic scars.
- Health conditions: Diabetes, thyroid disorders, and malnutrition can delay healing.
Evidence‑Based Scar Treatment Options
Non‑Surgical Methods
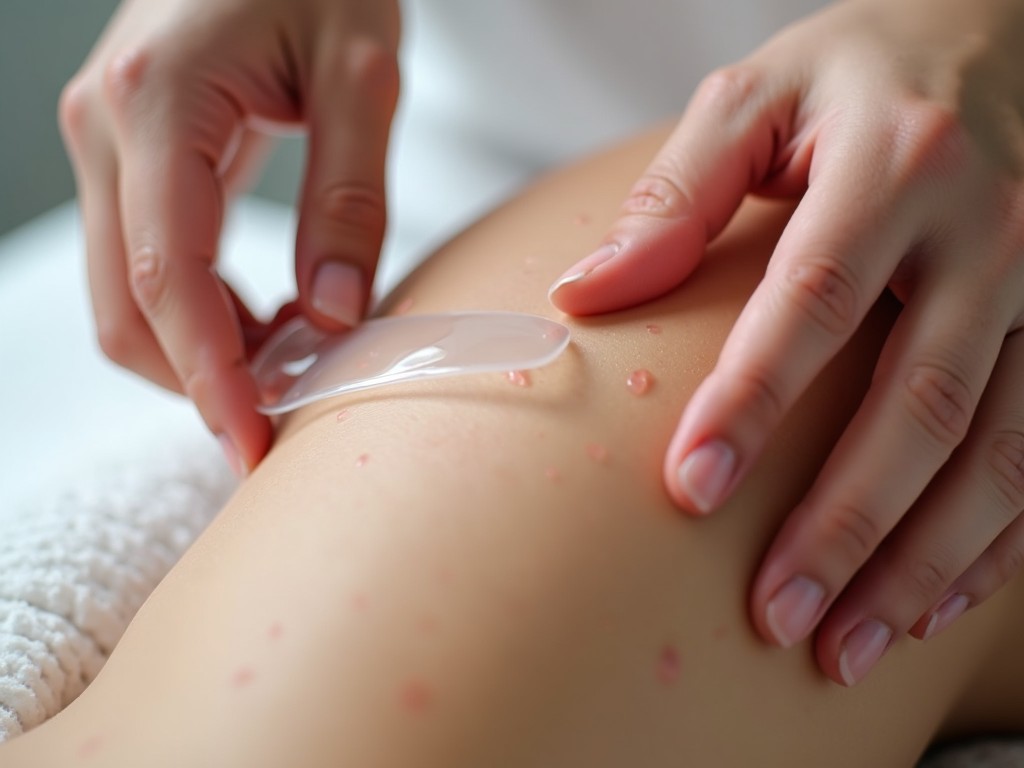
- Silicone Gel Sheets: Applied daily for 2–3 months; they hydrate the scar and reduce collagen overproduction.
- Silicone Gel Creams: Easier to apply, especially for irregular surfaces.
- Pressure Therapy: Custom‑made garments or bandages that apply constant pressure, useful for burn scars.
- Massage & Stretching: Gentle manipulation improves pliability and reduces fibrosis.
- Topical Treatments: Vitamin E, onion extract, and corticosteroid creams can help, though evidence varies.
Advanced Medical Interventions
- Laser Therapy: Ablative or fractional lasers reduce redness, flatten texture, and stimulate collagen remodeling.
- Microneedling: Creates micro‑channels that promote collagen production and improve scar appearance.
- Intralesional Steroid Injections: Reduce inflammation and collagen deposition in hypertrophic scars.
- Platelet‑Rich Plasma (PRP): Concentrated growth factors accelerate healing and improve scar quality.
- Dermal Grafting & Skin Substitutes: For extensive burns or surgical defects, thin dermal grafts can replace scar tissue.
When Surgery Is Needed
- Scar excision followed by meticulous re‑approximation of edges.
- Z‑plasty or W‑plasty techniques that redistribute tension.
- Use of local or free tissue flaps to cover large defects.
Practical Steps to Promote Scar Healing
- Keep the wound clean: Use sterile saline or mild antiseptic solutions.
- Apply appropriate dressings: Non‑adhesive, breathable materials reduce maceration.
- Protect from sun: Use SPF 50+ sunscreen and cover the area with clothing.
- Stay hydrated and maintain a balanced diet: Vitamins C and E, zinc, and protein support collagen synthesis.
- Follow your clinician’s schedule: Regular follow‑ups allow early detection of complications.
Frequently Asked Questions (FAQ)
Will a scar ever disappear completely?
Most scars fade significantly over 1–2 years but rarely vanish entirely. Light, superficial scars may become almost invisible, while deeper or hypertrophic scars usually remain visible.
Can I prevent a scar from forming?
While you cannot stop the healing process, early wound care, proper dressing, and avoiding tension can minimize scar depth and width.
Is silicone gel the best option for all scars?
Silicone is effective for many types of scars, especially hypertrophic and keloid scars. However, individual responses vary; a dermatologist can recommend the best regimen.
When should I consider surgical revision?
If a scar is causing functional impairment, significant cosmetic concern, or if it’s hypertrophic/keloid and unresponsive to conservative measures, surgical revision may be appropriate.
Conclusion
Scar treatment is a multidisciplinary endeavor that blends science, technology, and personalized care. By understanding the biology of wound healing, recognizing the factors that influence scar quality, and applying evidence‑based therapies—whether topical, laser, or surgical—you can dramatically improve both the appearance and comfort of your scars. Remember, patience is key: the remodeling phase can take up to two years, but with consistent care, the results are often worth the wait.