Cesarean Section: When, Why, and What to Expect – A Comprehensive Guide
When a pregnancy reaches its final stages, the world often imagines a gentle, natural birth. Yet, for many mothers, a cesarean section (C‑section) becomes the safest and most appropriate option. This guide dives deep into the reasons behind a C‑section, the procedure itself, recovery tips, and common questions—so you can make informed decisions and feel confident about the birthing journey.
What Is a Cesarean Section?
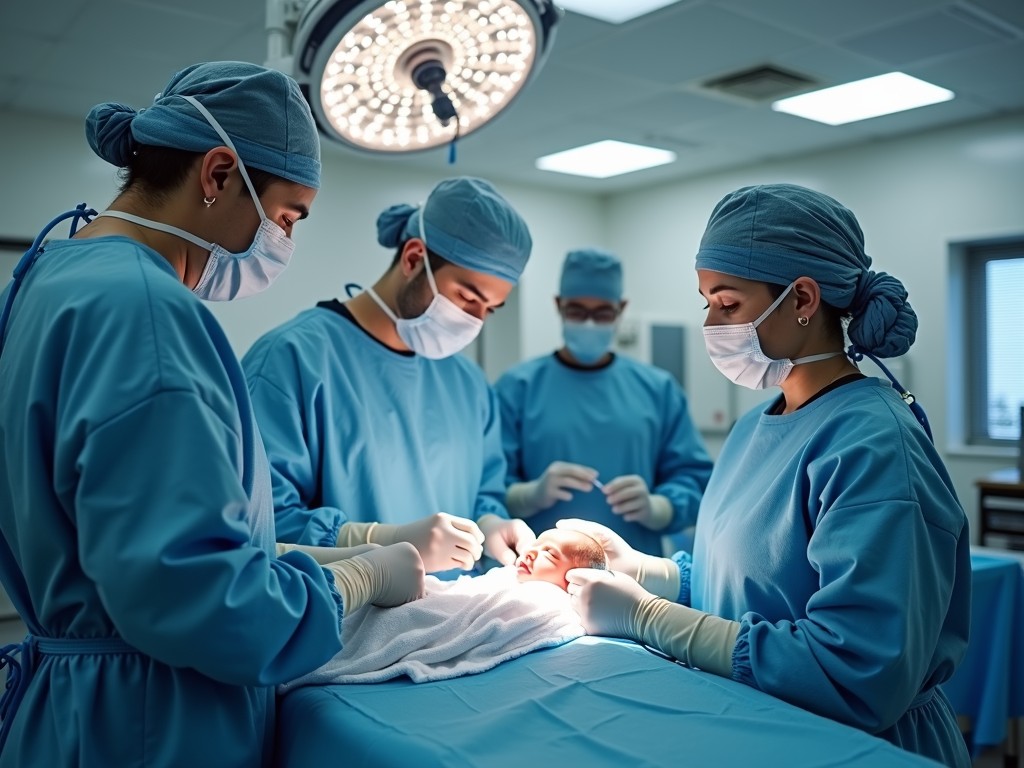
A cesarean section is a surgical delivery where the baby is delivered through an incision made in the mother’s abdomen and uterus. Unlike vaginal birth, the baby does not pass through the birth canal. The procedure is performed under anesthesia—usually spinal, epidural, or general—depending on the urgency and medical circumstances.
Why Do Doctors Recommend a C‑Section?
Over the past three decades, the rate of cesarean deliveries has risen worldwide—from around 10% to 35% in many regions. While some C‑sections are elective, most are medically indicated to protect the health of the mother and baby. Common indications include:
- Placenta Previa: The placenta covers the cervix, blocking the birth canal.
- Placental Abruption: The placenta detaches prematurely, causing bleeding and oxygen deprivation.
- Uterine Rupture: A tear in the uterus that can endanger both mother and child.
- Malpresentation: The baby’s position (e.g., breech or transverse lie) makes vaginal delivery risky.
- Fetal Distress: Reduced oxygen supply to the baby detected during monitoring.
- Maternal Health Conditions: Diabetes, hypertension, or infections like active genital herpes.
- Multiple Gestations: Twins or higher-order multiples often require a C‑section for safety.
- Previous C‑Section: About 90% of women who have had a C‑section will need another one.
The Cesarean Procedure Explained
The average surgery lasts about 45 minutes. Here’s a step‑by‑step overview:
- Preparation: The mother is given anesthesia and the abdomen is sterilized.
- Incision: A horizontal “bikini” cut is made in the lower abdomen; in emergencies, a vertical incision may be used.
- Uterine Opening: The uterine wall is carefully incised, usually in the lower segment.
- Delivery: The baby is gently lifted out, and the umbilical cord is clamped.
- Closure: The uterus, abdominal wall, and skin are sutured in layers.
- Post‑operative Care: Monitoring for bleeding, infection, and pain management.
Types of Anesthesia
- Spinal/Epidural: Common for planned C‑sections; offers pain relief while keeping the mother awake.
- General: Used in emergencies when rapid delivery is essential.
Recovery After a Cesarean Section
Recovery times vary, but most mothers can expect:
- Hospital stay of 2–4 days for uncomplicated cases.
- Gradual return to normal activities over 4–6 weeks.
- Potential for increased bleeding (average 600–800 mL) compared to vaginal birth.
- Risk of infection, blood clots, and adhesions that may affect future pregnancies.
Key post‑operative care tips:
- Keep the incision clean and dry.
- Use pain medication as prescribed.
- Walk regularly to promote circulation.
- Attend all follow‑up appointments.
- Seek immediate medical attention if you notice fever, excessive bleeding, or severe pain.
Common Questions About Cesarean Sections
Q: Can I have a vaginal birth after a C‑section (VBAC)?
A: Many women successfully have a VBAC, but it depends on the type of uterine incision, the reason for the previous C‑section, and overall health. Discuss with your obstetrician.
Q: Are there long‑term risks associated with C‑sections?
Yes. Potential risks include uterine rupture in future pregnancies, placenta previa, placenta accreta, and increased likelihood of cesarean in subsequent births.
Q: How does a C‑section affect breastfeeding?
Most mothers can breastfeed successfully after a C‑section. Early skin‑to‑skin contact and support from lactation consultants can help.
When to Call Your Doctor Immediately
Seek urgent care if you experience:
- Heavy vaginal bleeding (more than a pad per hour).
- Severe abdominal pain or fever.
- Rapid heart rate or dizziness.
- Any signs of infection (redness, swelling, foul odor).
Conclusion
A cesarean section is a life‑saving procedure that, when performed under proper medical guidance, offers a safe delivery for both mother and baby. Understanding the indications, the surgical process, and the recovery journey empowers expectant parents to make informed choices and prepare for a smooth postpartum experience. Remember, every birth story is unique—consult your healthcare provider to determine the best path for you and your little one.