Knee Replacement 101: What You Need to Know About Knee Arthroplasty and Prosthesis Care
Are you or a loved one battling chronic knee pain that limits daily activities? Knee replacement, also known as knee arthroplasty, offers a proven solution for severe osteoarthritis, rheumatoid arthritis, and traumatic joint damage. This guide breaks down the procedure, recovery, risks, and post‑operative care so you can make an informed decision and maximize the longevity of your knee prosthesis.
Understanding Knee Replacement
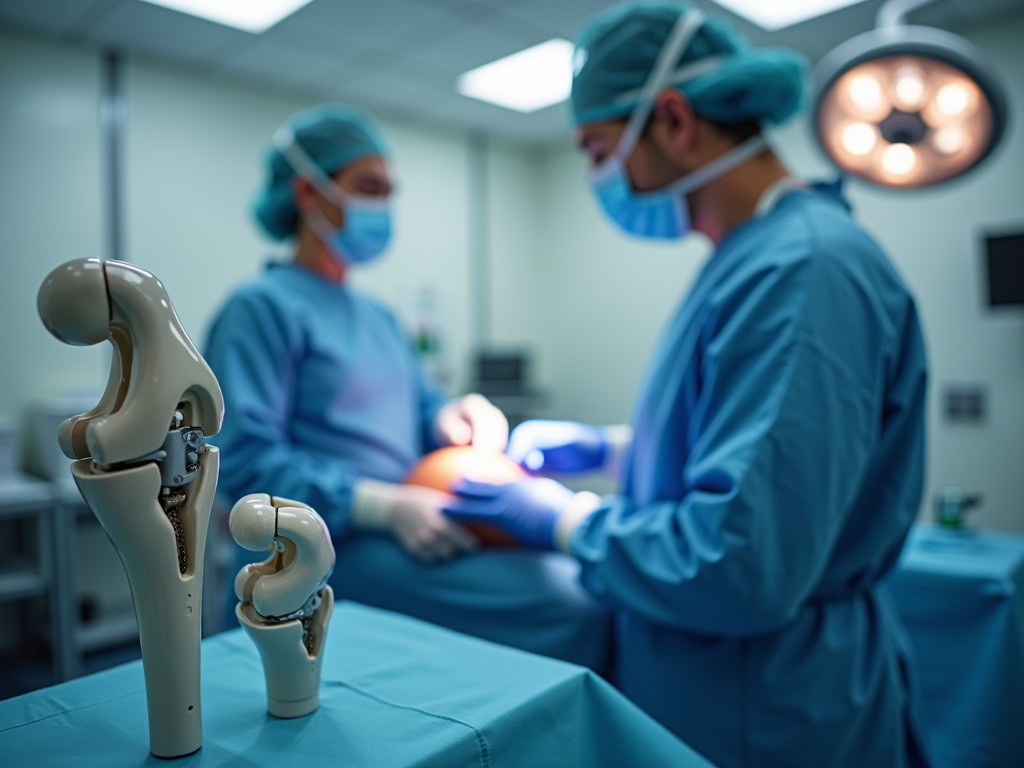
Knee arthroplasty replaces damaged cartilage and bone surfaces with durable metal and polyethylene components. The goal is to restore smooth joint motion, eliminate pain, and improve quality of life. Modern implants are engineered to mimic natural knee kinematics, providing a functional range of motion that closely resembles a healthy joint.
When Is Knee Replacement Indicated?
- Advanced osteoarthritis (gonarthrosis) – the most common reason for surgery.
- Rheumatoid arthritis – chronic inflammation that destroys joint structure.
- Post‑traumatic deformities – fractures or ligament injuries that lead to permanent joint damage.
- Severe knee deformity (varus/valgus) – long‑term misalignment causing uneven wear.
- Failed prior surgeries – unsuccessful arthroscopy or osteotomy may necessitate a prosthesis.
Who Is the Ideal Candidate?
Typically, patients over 55 with debilitating pain that interferes with walking, climbing stairs, or sitting for long periods are considered. Pain that persists even with medication and lifestyle changes, and a joint that shows significant cartilage loss on imaging, are key indicators.
The Knee Replacement Procedure
The operation usually lasts 1–2 hours and can be performed under spinal or general anesthesia. The surgeon makes a precise incision, removes the damaged bone and cartilage, and places the prosthetic components on the femur and tibia. In some cases, a polyethylene insert is added beneath the patella. A drain may be placed to prevent fluid buildup, and the incision is closed with sutures or staples.
Key Steps in the Surgery
- Incision and exposure of the knee joint.
- Resection of worn cartilage and bone surfaces.
- Preparation of femur and tibia for implant placement.
- Insertion of metal and polyethylene components.
- Optional patellar resurfacing.
- Closure, drain placement, and dressing.
Recovery and Rehabilitation
Recovery is a critical phase that determines the success of the implant. Early mobilization and structured physical therapy are essential for regaining strength and range of motion.
Immediate Post‑Op Care
- Patients are typically encouraged to stand the day after surgery.
- Pain management with medication and ice packs.
- Monitoring for signs of infection or blood clots.
Physical Therapy Milestones
- Weeks 1–2: Gentle knee flexion/extension exercises, ankle pumps, and use of a walker or cane.
- Weeks 3–6: Progress to independent walking, stair training, and strengthening of quadriceps and hamstrings.
- Months 3–6: Advanced strengthening, balance drills, and low‑impact activities such as stationary cycling or swimming.
- Beyond 6 months: Return to most daily activities; high‑impact sports usually remain contraindicated.
Typical Timeline
Full functional recovery often occurs within 3 months, but achieving the joint’s natural strength and flexibility can take up to 6 months. Consistent adherence to the rehab program is vital to prevent stiffness and ensure optimal implant performance.
Risks and Complications
While knee arthroplasty is generally safe, potential complications include:
- Infection at the surgical site.
- Blood clots (deep vein thrombosis or pulmonary embolism).
- Prosthesis loosening or wear over time.
- Joint stiffness or limited range of motion.
- Neural or vascular injury (rare).
Experienced surgeons and modern techniques significantly reduce these risks. Patients should maintain a healthy weight, avoid high‑impact activities, and attend regular follow‑ups to monitor implant integrity.
Post‑Operative Care and Lifestyle Tips
Maintaining the knee prosthesis involves more than just physical therapy. Here are practical guidelines to extend the life of your implant:
- Weight Management: Keep body weight within a healthy range to reduce joint load.
- Low‑Impact Exercise: Engage in activities like walking, cycling, or water aerobics.
- Avoid High‑Impact Sports: Running, jumping, or contact sports can accelerate wear.
- Regular Check‑Ups: Annual X‑rays and clinical evaluations help detect early loosening.
- Protective Gear: Use knee braces or supports during activities that pose a risk of falls.
Frequently Asked Questions
How long does a knee prosthesis last?
Modern implants typically last 15–20 years, though this can vary based on activity level, weight, and surgical technique.
Will I need to wear a brace after surgery?
Most patients do not require a brace once they regain sufficient strength and stability. However, a temporary brace may be prescribed during the early rehab phase.
Can I return to my job after knee replacement?
Many people resume normal work within 4–6 weeks, especially if the job is sedentary. Physical labor may require a longer recovery period.
Conclusion
Knee replacement offers a life‑changing solution for those suffering from severe joint degeneration. By understanding the surgical process, committing to a structured rehabilitation program, and adopting a joint‑friendly lifestyle, patients can enjoy pain‑free mobility and a durable prosthesis that lasts for decades. If you’re considering knee arthroplasty, consult with an experienced orthopedic surgeon to evaluate your candidacy and develop a personalized treatment plan.