Understanding Meniscus Tear Calcium Deposition: Causes, Symptoms, and Treatment Options
Meniscus tears are a common knee injury that can range from mild to severe. While most people associate a meniscus tear with sudden pain or swelling, a less-discussed factor—calcium deposition—can play a significant role in the development and progression of these injuries. In this comprehensive guide, we’ll explore how calcium deposits form in the meniscus, why they matter, and what you can do to prevent or manage this condition.
What Is a Meniscus Tear?
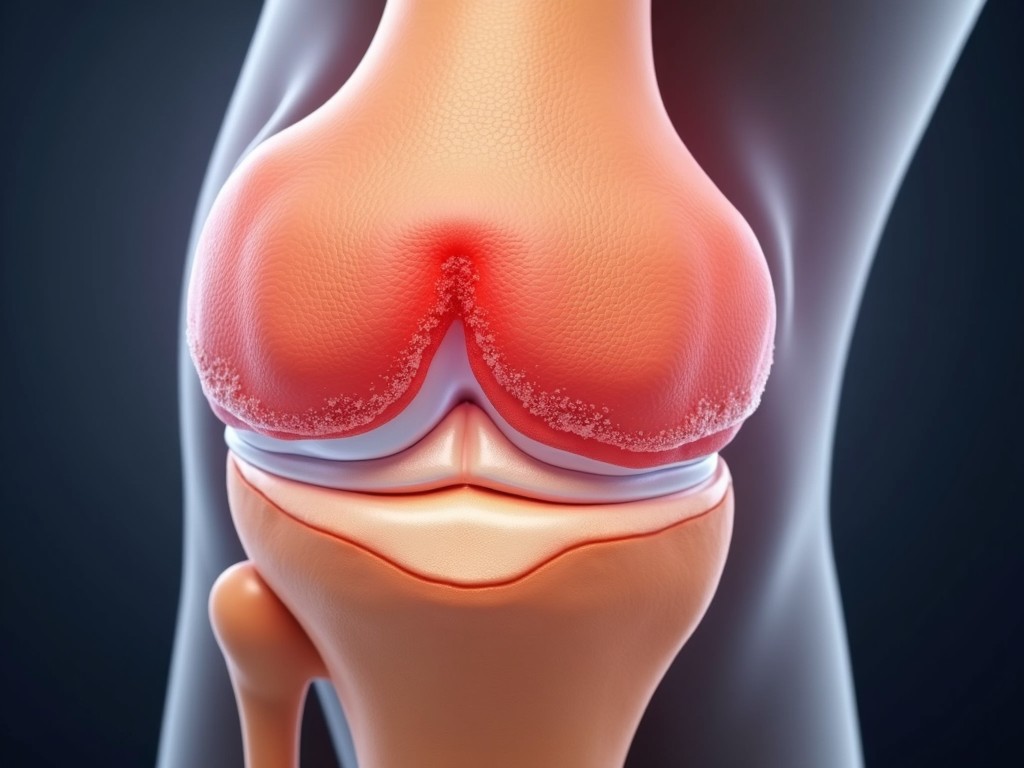
The meniscus is a C‑shaped cartilage disc that cushions the knee joint, distributing weight and stabilizing the joint. A tear can occur due to sudden twisting motions, repetitive stress, or degenerative wear and tear. Symptoms typically include pain, swelling, stiffness, and a feeling of the knee “locking.”
Calcium Deposition: The Hidden Culprit
Calcium deposition refers to the abnormal accumulation of calcium salts within the meniscal tissue. While the exact mechanism is still under investigation, several factors contribute to this process:
- Degenerative Changes: Age‑related wear can weaken the meniscus, making it more susceptible to calcium buildup.
- Inflammation: Chronic inflammation from repetitive injuries can alter the biochemical environment, encouraging calcium crystal formation.
- Metabolic Disorders: Conditions such as hyperparathyroidism or chronic kidney disease can increase serum calcium levels, promoting deposition in joint tissues.
- Trauma: A severe injury can trigger a cascade of cellular responses that lead to calcium precipitation.
Why Calcium Deposition Matters
When calcium crystals accumulate in the meniscus, they can:
- Reduce the cartilage’s elasticity, making it more prone to tears.
- Trigger localized inflammation, exacerbating pain and swelling.
- Complicate surgical repair by creating a less favorable tissue environment.
Recognizing the Signs of Calcium‑Related Meniscus Tears
While many symptoms overlap with typical meniscus tears, calcium deposition can intensify certain signs:
- Persistent, deep knee pain that doesn’t improve with rest.
- Visible swelling that appears suddenly after a minor injury.
- Stiffness that limits full range of motion.
- A sensation of “stuck” or “locked” knee during movement.
Diagnostic Tools
Accurate diagnosis is essential for effective treatment. Common methods include:
- Magnetic Resonance Imaging (MRI): Provides detailed images of cartilage and can detect calcium deposits.
- Ultrasound: Useful for evaluating soft tissue and identifying calcifications.
- Blood Tests: Assess calcium levels and rule out metabolic disorders.
- Arthroscopy: Allows direct visualization and removal of calcium deposits if necessary.
Treatment Options
Managing a meniscus tear with calcium deposition often requires a multi‑pronged approach:
- Conservative Care: Rest, ice, compression, and elevation (RICE), along with non‑steroidal anti‑inflammatory drugs (NSAIDs) to reduce pain and inflammation.
- Physical Therapy: Strengthening exercises for quadriceps and hamstrings to support the knee joint.
- Calcium‑Reducing Medications: In cases linked to metabolic disorders, treating the underlying condition can help lower calcium levels.
- Surgical Intervention: Arthroscopic removal of calcium deposits followed by meniscus repair or partial meniscectomy if the tear is extensive.
- Regenerative Therapies: Platelet‑rich plasma (PRP) or stem cell injections may promote cartilage healing.
Prevention Strategies
While not all meniscus tears are preventable, you can reduce your risk by:
- Maintaining a healthy weight to lessen joint load.
- Engaging in regular strength training to stabilize the knee.
- Warming up properly before sports or high‑impact activities.
- Addressing metabolic conditions promptly to keep calcium levels in check.
- Using proper footwear and knee supports during high‑risk activities.
Frequently Asked Questions
1. Can calcium deposition cause a meniscus tear?
Yes. Calcium deposits can weaken the meniscal tissue, making it more susceptible to tearing during normal or traumatic movements.
2. Is surgery always required for calcium‑related meniscus tears?
Not necessarily. Many cases respond well to conservative treatment, but surgery may be needed if the tear is large or if calcium deposits are causing significant inflammation.
3. How long does recovery take?
Recovery time varies. Conservative treatment may take 6–12 weeks, while surgical recovery can range from 3–6 months depending on the procedure and individual healing.
Conclusion
Meniscus tears are a common knee problem, but the added complexity of calcium deposition can worsen symptoms and complicate treatment. Early recognition, accurate diagnosis, and a tailored treatment plan—whether conservative or surgical—are key to restoring knee function and preventing future injuries. If you experience persistent knee pain or swelling, consult a healthcare professional for a thorough evaluation and personalized care plan.