Understanding Chronic Oral Conditions: Symptoms, Risks, and Prevention
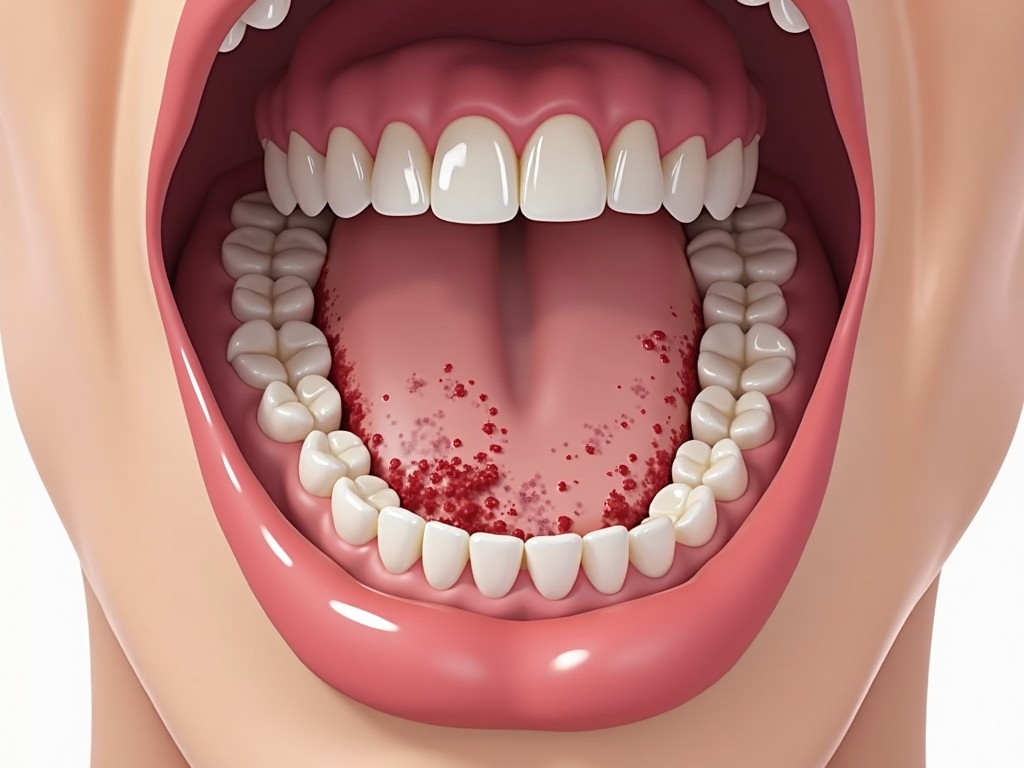
Chronic oral conditions can be subtle yet significant indicators of underlying health issues, including the risk of oral cancer. From white plaques to red ulcerations, these lesions often go unnoticed until they become painful or persistently troublesome. This guide provides a comprehensive overview of the most common chronic oral lesions, their causes, diagnostic approaches, and effective management strategies.
1. Common Chronic Oral Lesions
1.1 Leukoplakia
Leukoplakia presents as a persistent white patch on the oral mucosa that does not scrape off. It is often linked to chronic irritation from smoking, alcohol, or ill-fitting dentures. While benign, leukoplakia carries a potential for malignant transformation—especially lesions larger than 2.5 cm or those that are nodular. Early biopsy and regular monitoring are essential.
1.2 Lichen Planus
Primarily affecting women over 40, oral lichen planus shows irregular, erythematous borders with a yellowish, ulcerated base. The condition is immune‑mediated and can be associated with systemic autoimmune disorders. Though usually non‑cancerous, persistent lesions warrant biopsy to rule out dysplasia.
1.3 Candidiasis (Oral Thrush)
Caused by Candida albicans, candidiasis manifests as creamy white plaques that bleed when scraped. Risk factors include immunosuppression, diabetes, and prolonged antibiotic use. Antifungal therapy and addressing underlying conditions typically resolve the infection.
1.4 Oral Lichen Planus
Distinct from the skin variant, oral lichen planus can appear as white, lace‑like patterns or red, erosive lesions. It is often linked to stress and hormonal changes. Management focuses on topical steroids and maintaining oral hygiene.
1.5 Recurrent Aphthous Stomatitis
Commonly known as canker sores, these painful ulcers recur on the tongue, lips, or inside the cheeks. While usually benign, frequent episodes may indicate nutritional deficiencies or immune dysregulation.
1.6 Oral Melanoma and Other Pigmented Lesions
Dark spots or patches that change in size or color should be evaluated promptly. Oral melanoma is rare but aggressive; early detection improves prognosis.
2. Risk Factors for Chronic Oral Lesions and Oral Cancer
- Smoking and Tobacco Use – The leading cause of leukoplakia and oral cancer.
- Alcohol Consumption – Synergistic effect with tobacco increases malignant potential.
- HPV Infection – Associated with oral warts, condyloma acuminatum, and some oral cancers.
- Immunosuppression – Increases susceptibility to candidiasis and other opportunistic infections.
- Poor Oral Hygiene – Leads to chronic inflammation and ulceration.
- Ill‑fitting Prostheses – Causes mechanical trauma and chronic irritation.
- Genetic Predisposition – Family history of oral cancer raises risk.
3. Diagnosis: When to Seek Professional Care
Any oral lesion that persists for more than two weeks, changes in size or color, or is accompanied by pain, bleeding, or difficulty swallowing should be evaluated by a dentist or oral surgeon. Diagnostic steps include:
- Clinical Examination – Visual inspection and palpation.
- Biopsy – Gold standard for distinguishing benign from malignant lesions.
- Imaging – X‑ray, CT, MRI, or PET‑CT for assessing depth and spread.
- Laboratory Tests – Blood work for immune status, fungal cultures for candidiasis.
4. Treatment Options
4.1 Conservative Management
- Topical corticosteroids for lichen planus.
- Antifungal mouthwashes for candidiasis.
- Improved oral hygiene and removal of irritants.
- Dietary supplements for nutritional deficiencies.
4.2 Surgical Intervention
- Excisional biopsy for suspicious lesions.
- Laser therapy for small, well‑defined lesions.
- Resection for confirmed oral cancers.
4.3 Adjunctive Therapies
- Radiation therapy for advanced cancers.
- Systemic chemotherapy for metastatic disease.
- Immunotherapy for HPV‑related lesions.
5. Prevention and Lifestyle Modifications
- Quit smoking and avoid tobacco products.
- Limit alcohol intake.
- Maintain rigorous oral hygiene with fluoride toothpaste and regular dental visits.
- Ensure prostheses fit properly and are cleaned daily.
- Manage stress and maintain a balanced diet rich in vitamins.
- Vaccinate against HPV where applicable.
6. Frequently Asked Questions
Q: Can leukoplakia turn into cancer?
A: Yes, especially if the lesion is large, nodular, or fails to respond to treatment. Regular monitoring and biopsy are recommended.
Q: How often should I get a dental check‑up?
A: At least twice a year for routine cleaning and oral cancer screening.
Q: Are oral warts dangerous?
A: Most are benign, but HPV‑related warts can be precancerous. Early removal and monitoring are advised.
Conclusion
Chronic oral conditions, while often benign, can serve as early warning signs for more serious diseases, including oral cancer. Understanding the common lesions, recognizing risk factors, and seeking timely professional evaluation are key steps in preserving oral health. By adopting preventive measures—such as quitting smoking, maintaining excellent oral hygiene, and ensuring regular dental check‑ups—you can significantly reduce the risk of chronic lesions progressing to malignancy.