Varicose Veins Explained: Symptoms, Causes, Prevention & Treatment Options
Are those twisted blue veins on your legs more than just a cosmetic concern? Varicose veins are a common vascular condition that can affect anyone, regardless of age or gender. While many people dismiss them as a harmless aesthetic issue, untreated varicose veins can lead to pain, swelling, skin changes, and even serious complications such as ulcers or deep vein thrombosis. This comprehensive guide will walk you through the causes, symptoms, risk factors, prevention strategies, and the full spectrum of treatment options—so you can make informed decisions about your vascular health.
What Are Varicose Veins?
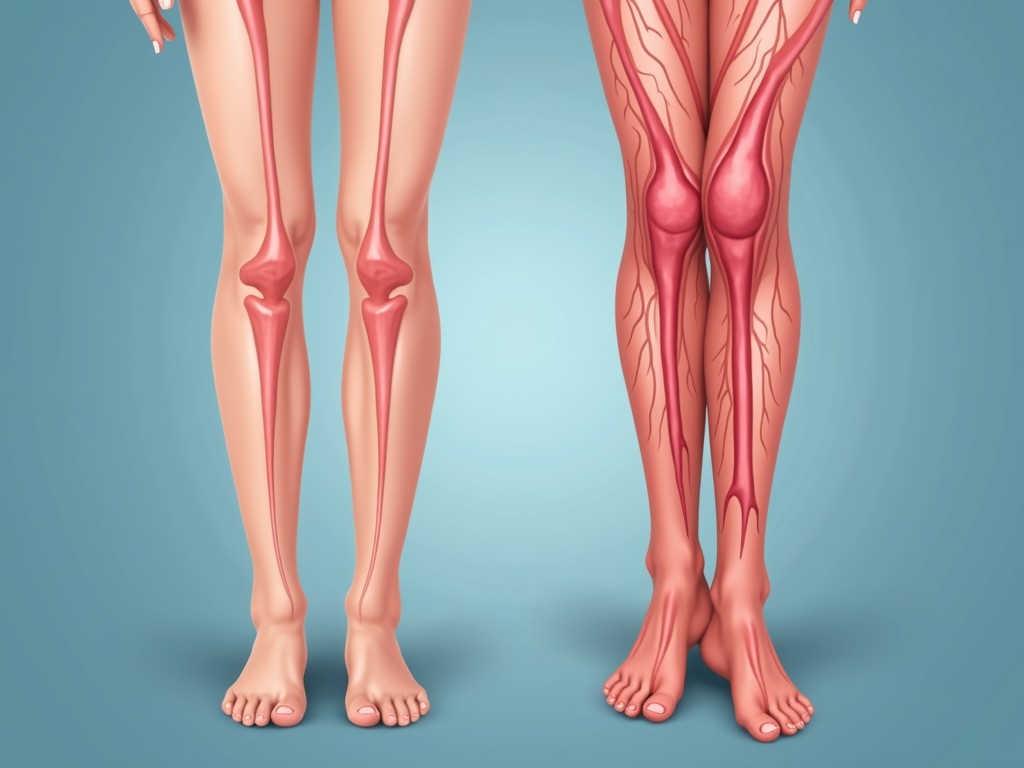
Varicose veins occur when the valves inside the veins fail to function properly, causing blood to pool and the veins to dilate. The condition is most commonly seen in the legs and feet, where the blood must travel against gravity to return to the heart. When the valves collapse, the veins become enlarged, twisted, and often visible just beneath the skin.
Key Symptoms & Signs
- Visible, blue or purple veins: Often twisted and prominent near the skin surface.
- Leg heaviness or aching: Worsens after prolonged standing or sitting.
- Swelling (edema): Especially in the lower legs and ankles.
- Itching, burning, or tingling: Around the affected veins.
- Skin changes: Darkening, dryness, or ulceration near the veins.
- Night cramps or numbness: Due to impaired blood flow.
Common Risk Factors
Understanding the risk factors can help you take preventive measures:
- Age: Vein walls lose elasticity over time.
- Gender: Women are more prone due to hormonal changes.
- Family history: Genetics play a role.
- Pregnancy: Increased blood volume and hormonal shifts.
- Obesity: Extra weight puts pressure on veins.
- Sedentary lifestyle: Long periods of sitting or standing.
- Smoking: Damages blood vessels.
- High‑heel footwear: Alters leg muscle function.
- Previous venous disorders: Such as deep vein thrombosis.
Prevention Tips: Keep Your Veins Healthy
- Exercise regularly: Walking, swimming, or cycling strengthens leg muscles and improves circulation.
- Maintain a healthy weight: Reduces pressure on the veins.
- Limit prolonged sitting or standing: Take short walks or stretch every 30 minutes.
- Wear supportive footwear: Avoid high heels; opt for flat or low‑heel shoes.
- Use compression stockings: Especially if you have a family history or spend long hours on your feet.
- Elevate your legs: When resting, lift your legs above heart level to aid blood flow.
- Stay hydrated and reduce salt intake: Helps prevent fluid retention.
- Quit smoking: Improves overall vascular health.
Varicose Vein Treatment Options
Treatment depends on the severity, type of veins involved, and overall health. Options range from conservative measures to minimally invasive procedures and surgery.
1. Conservative Management
- Compression stockings: Apply gentle pressure to improve venous return.
- Exercise & lifestyle changes: Strengthen calf muscles and reduce risk factors.
- Dietary adjustments: High‑fiber foods, omega‑3 fatty acids, and antioxidants support vein health.
2. Sclerotherapy
Suitable for small to medium surface veins. A sclerosant solution is injected into the vein, causing it to scar and close. The body then absorbs the treated vein over time.
3. Endovenous Laser Therapy (EVLT)
Laser energy is delivered through a fiber inserted into the vein, heating and sealing it shut. This minimally invasive option is effective for larger surface veins.
4. Radiofrequency Ablation (RFA)
Similar to laser therapy but uses radiofrequency energy to heat and close the vein.
5. Ambulatory Phlebectomy
Small incisions are made to remove superficial veins. It’s often combined with other procedures for optimal results.
6. Surgical Stripping
Reserved for severe cases. The affected vein is removed or ligated through a small incision. Recovery time is longer compared to minimally invasive methods.
Post‑Treatment Care & Recovery
After any procedure, follow your doctor’s instructions closely:
- Wear compression stockings as prescribed.
- Avoid heavy lifting and strenuous exercise for the recommended period.
- Keep the treated area clean and monitor for signs of infection.
- Attend all follow‑up appointments to ensure proper healing.
Frequently Asked Questions
Q: Are varicose veins only a cosmetic issue?
A: No. While they can be unsightly, varicose veins can cause pain, swelling, skin ulcers, and increase the risk of blood clots.
Q: Can pregnancy cause varicose veins?
A: Yes. Hormonal changes and increased blood volume during pregnancy can lead to vein dilation.
Q: When should I see a doctor?
Seek medical advice if you experience severe pain, skin changes, swelling, or if you have a family history of venous disease.
Q: Are there natural remedies?
While lifestyle changes help, there is limited scientific evidence for herbal or alternative treatments. Always consult a healthcare professional before trying new remedies.
Conclusion
Varicose veins are more than a cosmetic concern—they can impact your comfort, mobility, and overall health. By recognizing the symptoms early, understanding your risk factors, and adopting preventive habits, you can reduce the likelihood of developing severe varicose veins. If you already have visible veins, a range of effective treatments—from compression stockings to laser therapy—can restore both function and confidence. Remember, early intervention is key: schedule a consultation with a vascular specialist if you notice any changes in your legs, and take proactive steps to protect your veins for a healthier future.