Varicose Veins: Symptoms, Causes, and Effective Treatment & Prevention Tips
Varicose veins are often dismissed as a purely cosmetic issue, but they can cause significant discomfort and even serious health complications. If you notice swollen, bulging veins in your legs, feel a heavy or aching sensation, or experience itching and skin changes, you might be dealing with varicose veins. This guide dives deep into the symptoms, causes, and practical steps you can take to manage and prevent varicose veins, ensuring you stay healthy and confident.
What Are Varicose Veins?
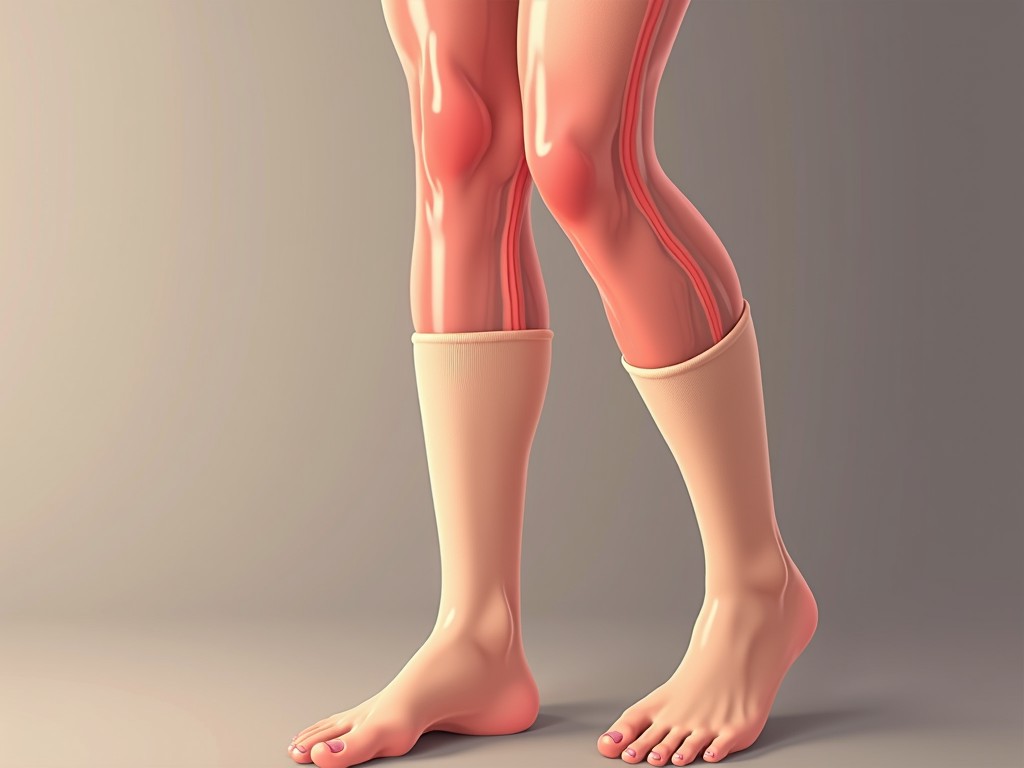
Varicose veins are enlarged, twisted veins that usually appear in the lower extremities. They result from weakened valves and walls in the veins, which allow blood to pool and the veins to dilate. While many people view them as a cosmetic concern, the condition can lead to pain, swelling, skin changes, and in severe cases, ulcers or blood clots.
Common Symptoms of Varicose Veins
Recognizing the signs early can help you seek treatment before complications arise. Here are the most frequently reported symptoms:
- Visible, bulging veins: Often purple, blue, or red, these veins may form a knot-like pattern and feel tender under the skin.
- Pain and discomfort: A heavy, aching, or throbbing sensation that worsens after prolonged standing or sitting.
- Swelling (edema): Noticeable puffiness in the legs, especially after a long day or when lying down for extended periods.
- Itching or skin changes: Irritation, redness, or darkened patches around the affected veins.
- Bleeding: Minor cuts or abrasions over varicose veins can bleed more easily due to fragile skin.
- Muscle cramps and numbness: Tingling or numbness in the legs, often occurring at night or after inactivity.
- Cosmetic concerns: Visible veins can affect self-esteem and confidence.
Why Do Varicose Veins Develop?
Several factors contribute to the development of varicose veins:
- Genetics: A family history of varicose veins increases risk.
- Age: Vein walls weaken over time.
- Gender: Women are more prone, possibly due to hormonal changes during pregnancy and menopause.
- Pregnancy: Increased blood volume and hormonal shifts can strain veins.
- Obesity: Extra weight adds pressure to leg veins.
- Prolonged standing or sitting: Poor circulation can lead to valve failure.
- Smoking: Damages blood vessels and impairs circulation.
Effective Treatment Options
Treatment depends on severity, symptoms, and overall health. Options range from lifestyle changes to medical procedures:
1. Lifestyle Modifications
- Regular exercise: Low-impact activities like walking, cycling, and swimming strengthen leg muscles and improve blood flow.
- Leg elevation: Raising legs above heart level for 15–20 minutes several times a day reduces swelling.
- Avoid prolonged standing or sitting: Take short walks or stretch every 30–60 minutes.
- Maintain a healthy weight: Reduces pressure on veins.
- Quit smoking: Improves vascular health.
- Compression stockings: Provide graduated pressure to keep veins from dilating.
- Cold compress: Can relieve pain and reduce swelling.
- Stress management: Techniques like yoga, meditation, or deep breathing can help.
2. Medical Interventions
- Conservative procedures: Sclerotherapy, laser therapy, or radiofrequency ablation are minimally invasive options that close or shrink varicose veins.
- Invasive procedures: Endovenous laser treatment (EVLT) or ambulatory phlebectomy may be recommended for larger veins.
- Medication: Certain drugs can reduce inflammation and improve vein tone.
- Follow-up care: Regular check-ups ensure early detection of recurrence.
Prevention Strategies
While genetics play a role, many risk factors are modifiable. Here’s how you can reduce your chances of developing varicose veins:
- Exercise regularly and keep your legs active.
- Elevate your legs whenever possible.
- Maintain a healthy weight.
- Wear compression stockings if you’re at high risk.
- Avoid tight clothing that restricts circulation.
- Quit smoking and limit alcohol intake.
- Use proper footwear with good arch support.
- Stay hydrated and eat a balanced diet rich in fiber.
Frequently Asked Questions
Do varicose veins always require treatment?
Not always. If they’re asymptomatic and not causing discomfort, many people choose to monitor them. However, if you experience pain, swelling, or skin changes, treatment is advisable.
Can varicose veins lead to serious health problems?
Yes. Complications can include skin ulcers, blood clots (deep vein thrombosis), and chronic venous insufficiency. Early intervention can prevent these outcomes.
Are compression stockings effective?
Compression stockings are highly effective in reducing symptoms and preventing progression, especially when worn consistently during the day.
What’s the difference between varicose veins and spider veins?
Spider veins are smaller, superficial veins that appear as fine lines, whereas varicose veins are larger, bulging veins that often cause discomfort.
Conclusion
Varicose veins are more than a cosmetic issue—they can impact your quality of life and overall health. By recognizing early symptoms, adopting preventive measures, and seeking appropriate treatment, you can manage the condition effectively. If you notice any of the symptoms listed above, consult a healthcare professional for a personalized assessment and treatment plan. Remember, early action is key to preventing complications and maintaining healthy circulation.