Varicocele: When Is Treatment Really Needed? A Comprehensive Guide to Diagnosis, Treatment, and Outcomes
Varicocele is one of the most common reversible causes of male infertility, yet many men wonder whether surgery is always necessary. This guide breaks down the facts—prevalence, side‑specific differences, surgical options, potential complications, and clear indications for treatment—so you can make an informed decision about your reproductive health.
What Is a Varicocele?
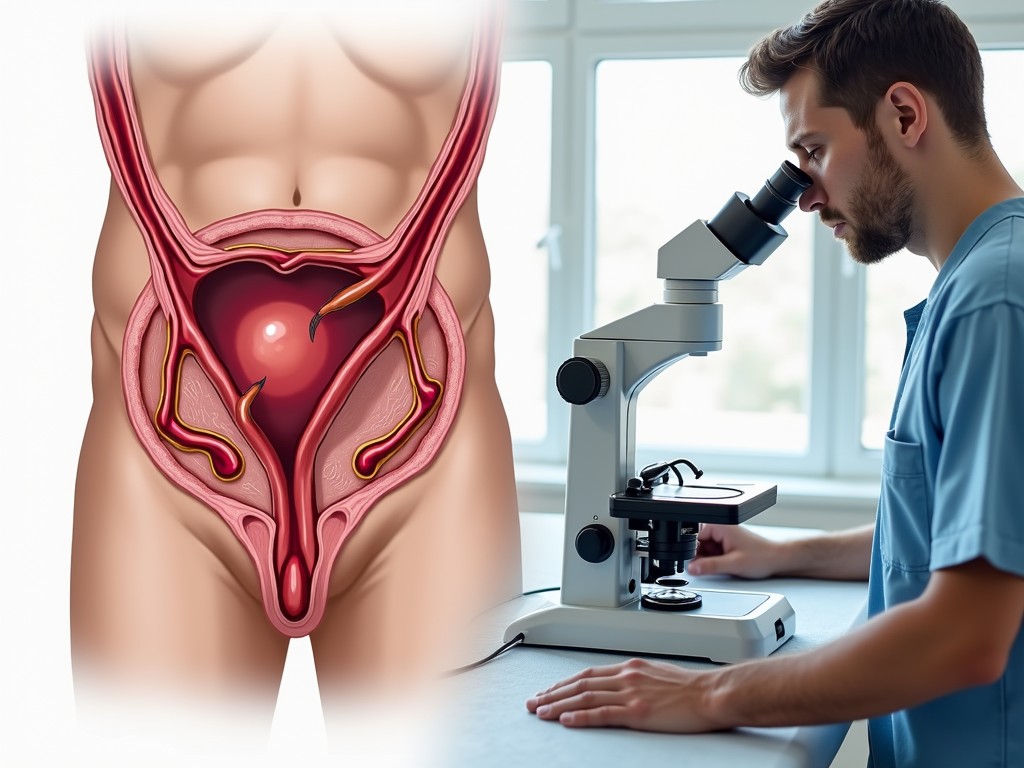
A varicocele is an abnormal dilation of the pampiniform plexus veins surrounding the testicle. Think of it as a “varicose vein” in the scrotum. It can impair sperm production and hormone synthesis, leading to infertility or testicular pain.
How Common Is It?
- Occurs in about 15% of all men.
- In men who seek medical care for infertility, the prevalence rises to roughly 40%.
- Most cases develop during adolescence; it is rare in children under 10.
Why Does It Usually Affect the Left Side?
The left testicular vein drains into the left renal vein at a higher angle, making it more susceptible to blood stasis. Consequently, left‑sided varicoceles are far more common than right‑sided ones. When a right‑sided varicocele is present, clinicians should evaluate for possible renal or pelvic masses that could be obstructing venous flow.
Varicocele Surgery (Varicocelectomy): What You Need to Know
The standard surgical procedure is called varicocelectomy. While it is generally low‑risk, the technique used can dramatically influence outcomes.
Microsurgical vs. Conventional Techniques
Microsurgical varicocelectomy uses an operating microscope to identify and ligate tiny veins while preserving arteries and lymphatics. This precision reduces:
- Recurrence (re‑varicocele)
- Hydrocele formation
- Testicular atrophy
- Neurovascular injury
Conventional methods, lacking magnification, carry higher rates of these complications.
Potential Complications
- Recurrence: Failure to ligate small veins can lead to re‑varicocele.
- Hydrocele: Damage to lymphatics may cause fluid accumulation.
- Testicular atrophy: Accidental arterial injury can shrink the testicle.
- Neurovascular injury: Nerve or vas deferens damage may cause numbness or fertility issues.
When Is Varicocele Surgery Indicated?
Not every varicocele requires surgery. The decision hinges on a combination of clinical findings, semen analysis, and patient goals.
Infertility-Related Indications
- Abnormal sperm count, motility, or morphology.
- Normal sperm parameters but a history of infertility.
- Men planning to conceive in the near future.
- Couples with unexplained infertility where varicocele is the only identified abnormality.
Pain Management
Chronic scrotal pain that does not respond to analgesics, scrotal elevation, or other conservative measures may be relieved by varicocelectomy, even if sperm parameters are normal.
Other Considerations
- Adolescent patients with testicular size discrepancy.
- Men with low testosterone levels attributable to varicocele.
- Patients with a history of testicular trauma or surgery where varicocele may have developed.
Pre‑operative Evaluation
Before surgery, a thorough assessment is essential:
- Scrotal Doppler ultrasound to confirm varicocele and rule out other pathologies.
- Semen analysis (at least two samples) to document baseline parameters.
- Hormonal profile (testosterone, LH, FSH) if low testosterone is suspected.
- Partner evaluation to exclude female infertility factors.
Post‑operative Expectations
Most patients experience:
- Improved sperm count and motility within 3–6 months.
- Reduction or resolution of scrotal pain.
- Potential increase in testosterone levels.
- Low recurrence rates with microsurgical technique (<5%).
Frequently Asked Questions
Is varicocele always a cause of infertility?
No. While varicoceles are common in infertile men, many men with varicoceles have normal sperm parameters. Treatment is usually reserved for those with documented fertility issues.
Can varicocele surgery be performed on a single testicle?
Yes. Unilateral varicocelectomy is common, especially when only one side is affected. Bilateral surgery is considered if both sides are symptomatic or if the contralateral side is at risk.
What is the recovery time after microsurgical varicocelectomy?
Most men return to normal activities within 1–2 weeks. However, full recovery of sperm parameters may take up to 6 months.
Are there non‑surgical alternatives?
Conservative measures (scrotal support, pain medication) can alleviate discomfort but do not correct the underlying venous dilation. They are not effective for improving fertility.
Conclusion
Varicocele is a common, treatable condition that can impact fertility and cause chronic pain. However, surgery is not mandatory for every case. A careful evaluation of semen parameters, hormonal status, and patient goals—combined with a high‑quality microsurgical approach—offers the best chance for improved outcomes and reduced complications. If you suspect a varicocele or are experiencing infertility, consult a urologist for a comprehensive assessment and personalized treatment plan.