Proctology Explained: Diagnosis, Treatment, and Prevention of Anorectal Health Issues
Proctology is a specialized branch of medicine that focuses on the diagnosis, treatment, and management of diseases affecting the anorectal region. From common conditions like hemorrhoids and anal fissures to more serious concerns such as colorectal cancer, proctology plays a vital role in preserving quality of life and preventing serious complications. In this comprehensive guide, we’ll explore what proctology entails, the most common anorectal disorders, diagnostic tools, cutting‑edge treatments, and practical prevention strategies.
What Is Proctology?
Proctology, also known as anorectal surgery, deals with disorders of the rectum, anus, and surrounding tissues. Proctologists are trained to perform physical examinations, interpret imaging studies, and provide both medical and surgical interventions. The field covers a wide spectrum of conditions, including:
- Hemorrhoids (internal and external)
- Anal fissures and fistulas
- Anal abscesses and cysts
- Anal warts (HPV-related)
- Colorectal and anal cancers
- Inflammatory bowel disease (Crohn’s, ulcerative colitis)
- Diverticulitis, constipation, and diarrhea
- Irritable bowel syndrome (IBS)
Why Proctology Matters
Disorders of the anorectal region can severely impact daily life, causing pain, bleeding, and embarrassment. Early detection and treatment are essential to:
- Reduce pain and discomfort
- Prevent complications such as infection or bleeding
- Detect early signs of colorectal cancer
- Improve overall quality of life
Diagnostic Tools in Proctology
Physical Examination
Proctologists perform a thorough rectal exam, often using a proctoscope to visualize the anal canal and lower rectum.
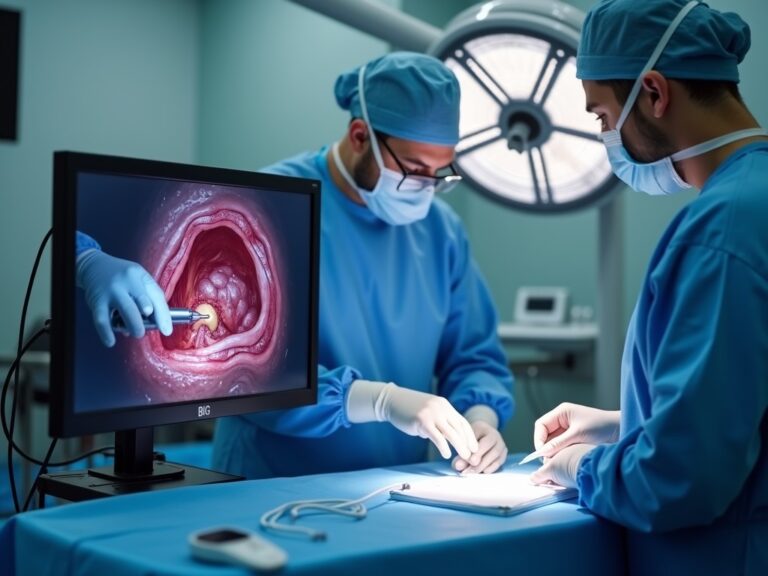
Imaging and Endoscopy
- Sigmoidoscopy – examines the sigmoid colon and rectum.
- Colonoscopy – full colon evaluation, essential for cancer screening.
- Anorectal Manometry – measures sphincter pressure and function.
- Ultrasound and MRI – detailed imaging of fistulas and abscesses.
Common Anorectal Conditions and Their Management
Hemorrhoids
Swollen veins in the rectal area can cause itching, pain, and bleeding. Treatment options range from lifestyle changes to minimally invasive procedures:
- Dietary fiber and hydration
- Topical creams and suppositories
- Rubber band ligation
- Infrared coagulation
- Laser therapy
- Transanal hemorrhoidectomy (for severe cases)
Anal Fissures
Small tears in the anal lining often result from hard stools. Management includes:
- High‑fiber diet and stool softeners
- Topical nitroglycerin or calcium channel blockers
- Botox injections to relax the sphincter
- In severe, surgical repair (lateral internal sphincterotomy)
Anal Fistulas and Abscesses
Fistulas are abnormal tunnels between the anal canal and perianal skin, often following an abscess. Treatment typically involves:
- Incision and drainage of abscesses
- Seton placement to allow gradual closure
- Fistulotomy or advancement flap procedures
- Use of fibrin glue or plugs in selected cases
Anal Cancer and Colorectal Cancer
Early detection is critical. Screening methods include colonoscopy and fecal occult blood tests. Treatment may involve:
- Endoscopic mucosal resection (EMR)
- Transanal endoscopic microsurgery (TEM)
- Radiation therapy
- Systemic chemotherapy
- Surgical resection (low anterior resection, abdominoperineal resection)
Innovations in Proctology Treatment
Recent advances have made procedures less invasive and more patient‑friendly:
- Laser Therapy – precise coagulation with minimal pain.
- Infrared Coagulation – effective for internal hemorrhoids.
- Robotic Surgery – enhanced dexterity for complex anorectal procedures.
- High‑Resolution Anorectal Manometry – better assessment of sphincter function.
- Improved imaging (3‑D MRI) for detailed fistula mapping.
Prevention Strategies for Anorectal Health
Adopting healthy habits can significantly reduce the risk of proctologic disorders:
- Consume a fiber‑rich diet (whole grains, fruits, vegetables).
- Stay hydrated – aim for 8–10 glasses of water daily.
- Exercise regularly to promote bowel motility.
- Avoid prolonged sitting; take short breaks to move.
- Practice proper toileting habits – don’t strain.
- Use stool softeners or fiber supplements if constipation is chronic.
- Get regular colorectal cancer screening after age 45 (or earlier if risk factors).
Frequently Asked Questions
What are the early signs of hemorrhoids?
Common symptoms include itching, bright red bleeding during bowel movements, and a feeling of fullness or a lump near the anus.
When should I see a proctologist?
If you experience persistent rectal pain, bleeding, or changes in bowel habits, or if you have a family history of colorectal cancer, schedule an appointment.
Are proctology procedures painful?
Most minimally invasive procedures are performed under local or general anesthesia and are associated with minimal postoperative pain. Recovery times vary but are typically short.
Can lifestyle changes cure anal fissures?
In many cases, dietary changes, stool softeners, and topical treatments can heal fissures. However, chronic fissures may require surgical intervention.
Conclusion
Proctology is a critical field that addresses a wide range of anorectal conditions, from everyday discomforts to life‑threatening cancers. By understanding the signs, seeking timely diagnosis, and embracing modern treatment options, patients can achieve relief and maintain a high quality of life. If you notice any symptoms related to the anorectal region, don’t delay – consult a qualified proctologist for a thorough evaluation and personalized care plan.