Jaw Pain Explained: Causes, Symptoms, and Effective Treatment Options
Jaw pain can turn everyday activities—eating, speaking, even sleeping—into uncomfortable challenges. Whether you’re dealing with a dull ache or a sharp, throbbing pain, understanding the root causes and available treatments is essential for regaining comfort and confidence. This guide dives deep into the most common triggers of jaw pain, the science behind temporomandibular joint (TMJ) disorders, and practical steps you can take to find relief.
What Is Jaw Pain and Why Does It Matter?
Jaw pain, medically referred to as mandibular pain, often signals an underlying issue that can range from dental problems to joint inflammation. Left untreated, chronic jaw discomfort can lead to headaches, ear pain, and even affect posture and sleep quality. Recognizing early warning signs and seeking timely care can prevent complications and improve quality of life.
Common Causes of Jaw Pain
1. Dental Issues
Tooth decay, gum disease, and misaligned teeth are frequent culprits. When a tooth is infected or a cavity is deep, the pain can radiate to the jaw joint. Bruxism—nighttime teeth grinding—places excessive pressure on the jaw, causing inflammation and soreness.
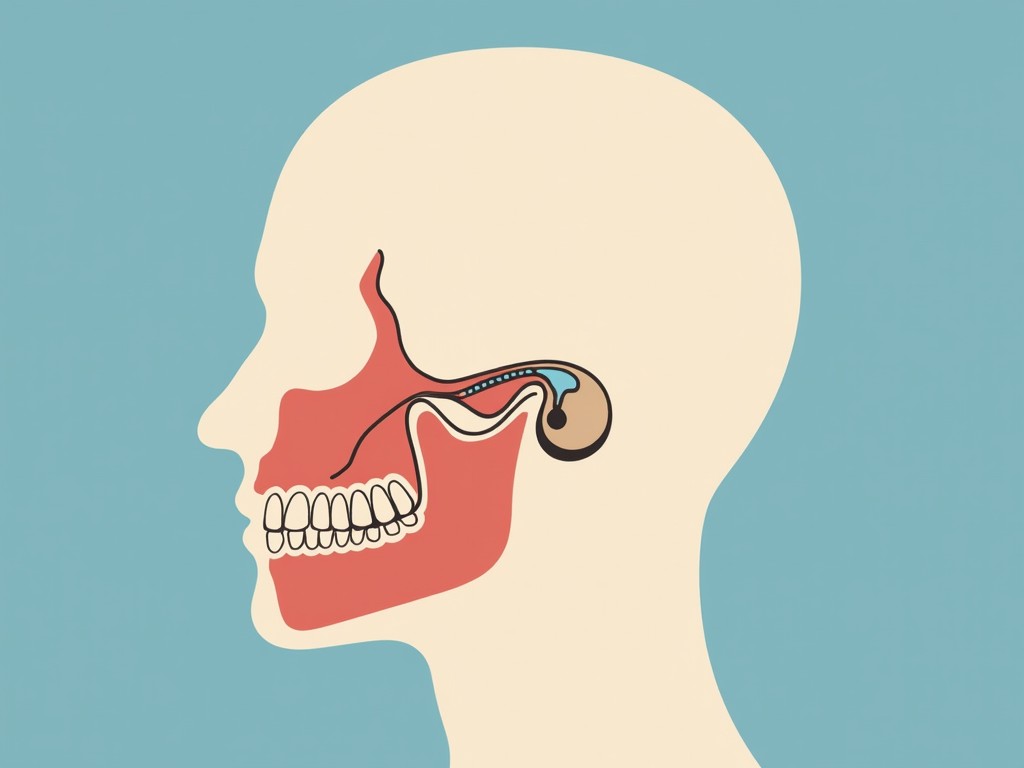
2. Temporomandibular Joint (TMJ) Disorders
The TMJ connects the lower jaw to the skull. Disorders such as temporomandibular joint dysfunction (TMD) can result in clicking sounds, limited mouth opening, and persistent pain. TMD often stems from joint misalignment, arthritis, or trauma.
3. Nerve Compression
Compression of facial nerves, especially the trigeminal nerve, can produce sharp, shooting pain in the jaw area. This may occur due to inflammation, tumors, or congenital abnormalities.
4. Stress and Muscle Tension
High stress levels trigger muscle tightening around the jaw. Over time, chronic tension can lead to myofascial pain syndrome, where trigger points in the jaw muscles cause persistent discomfort.
5. Arthritis and Inflammatory Conditions
Rheumatoid arthritis or osteoarthritis can affect the TMJ, leading to joint swelling, stiffness, and pain. Inflammatory markers in the joint fluid often indicate the severity of the condition.
Recognizing the Symptoms of TMJ Disorders
- Jaw pain or tenderness around the ear
- Clicking or popping sounds when opening or closing the mouth
- Limited jaw movement or difficulty chewing
- Headaches, especially at the temples or behind the eyes
- Earaches or a feeling of fullness in the ears
- Facial pain that radiates to the neck or shoulders
Diagnostic Pathways: How Doctors Identify the Root Cause
Diagnosing jaw pain typically involves a combination of:
- Comprehensive dental examination
- Physical assessment of jaw movement and muscle tone
- Imaging studies such as X-rays, CT scans, or MRI to visualize joint structures
- Blood tests to rule out inflammatory or autoimmune conditions
- Referral to an oral and maxillofacial specialist if complex issues arise
Treatment Options: From Home Care to Professional Interventions
1. Lifestyle Modifications
- Maintain proper posture to reduce strain on the jaw and neck
- Incorporate a balanced diet with soft foods during flare-ups
- Practice stress-reduction techniques such as meditation, yoga, or deep-breathing exercises
- Avoid chewing gum or hard candies that exacerbate jaw tension
2. Physical Therapy and Exercises
Targeted jaw exercises can strengthen muscles, improve joint mobility, and reduce pain. A physiotherapist may guide you through:
- Gentle stretching routines for the jaw and neck
- Isometric exercises to build muscle endurance
- Manual therapy techniques to release trigger points
3. Dental Interventions
- Nighttime occlusal splints (mouth guards) to prevent teeth grinding
- Corrective orthodontic treatment for misaligned teeth
- Root canal therapy or extraction for infected teeth causing pain
- Restorative procedures such as crowns or fillings to eliminate cavities
4. Pharmacologic Management
Over-the-counter pain relievers (NSAIDs) can alleviate inflammation. In more severe cases, doctors may prescribe muscle relaxants, low-dose antidepressants, or topical analgesics.
5. Advanced Therapies
- Injections of corticosteroids or hyaluronic acid into the TMJ to reduce inflammation
- Botulinum toxin (Botox) injections to relax overactive jaw muscles
- Surgical options such as arthroscopy or joint replacement for refractory cases
When to Seek Professional Help
If you experience:
- Persistent jaw pain lasting more than a few weeks
- Difficulty opening your mouth fully
- Severe headaches or ear pain accompanying jaw discomfort
- Visible swelling or redness around the jaw joint
- Any sudden changes in vision or facial numbness
Prompt evaluation by a dentist or oral surgeon can prevent chronic complications and guide you toward the most effective treatment plan.
Frequently Asked Questions (FAQ)
Q: Can stress alone cause jaw pain?
A: Yes. Stress triggers muscle tension and bruxism, which can lead to TMJ dysfunction and jaw pain.
Q: Are there natural remedies for jaw pain?
Natural approaches such as warm compresses, gentle stretching, and anti-inflammatory diets can provide relief, but they should complement, not replace, professional care.
Q: How long does it take to recover from TMJ disorder?
Recovery varies. Mild cases may improve within weeks with conservative therapy, while severe TMD may require months of treatment and lifestyle changes.
Conclusion
Jaw pain is more than a minor inconvenience—it can signal dental problems, joint disorders, or systemic conditions that warrant attention. By recognizing the common causes, seeking timely diagnosis, and embracing a multidisciplinary treatment approach—ranging from lifestyle tweaks to advanced medical interventions—you can reclaim comfort and prevent long-term damage. Remember, early intervention is key: if jaw pain persists or worsens, consult a qualified dental or medical professional to tailor a plan that addresses your unique needs.