Vertigo Diagnosis 101: How to Identify and Evaluate Balance Disorders
Vertigo is more than just a dizzy feeling—it’s a symptom that can signal a range of inner‑ear or neurological problems. If you or someone you know experiences sudden spinning sensations, knowing how to diagnose vertigo accurately is essential for effective treatment. This guide walks you through the diagnostic process, from patient history to advanced vestibular testing, so you can understand what doctors look for and why it matters.
What Is Vertigo and Why Accurate Diagnosis Matters
Vertigo is the medical term for the sensation that you or your surroundings are spinning. While it often stems from inner‑ear issues, it can also arise from central nervous system disorders. Misdiagnosing vertigo can lead to ineffective treatments, prolonged symptoms, and unnecessary anxiety. A thorough diagnostic work‑up helps pinpoint the exact cause—whether peripheral or central—so that the right therapy can be applied.
Types of Vertigo: Peripheral vs. Central
Understanding the two main categories of vertigo is the first step in diagnosis:
- Peripheral Vertigo – Most common; originates in the inner ear’s vestibular system. Symptoms often include hearing loss, tinnitus, and vertigo triggered by head movements.
- Central Vertigo – Arises from brainstem or cerebellar lesions. Symptoms may be accompanied by neurological deficits such as weakness, numbness, or visual disturbances.
Distinguishing between these types guides the choice of tests and treatment plans.
Step 1: Comprehensive Patient History (Anamnesis)
The first and most valuable tool in diagnosing vertigo is a detailed patient interview. Key questions include:
- When did the vertigo start? How long does each episode last?
- What triggers the dizziness? (e.g., head movement, lying down, stress)
- Are there accompanying symptoms? (hearing loss, tinnitus, headache, nausea)
- Any history of ear infections, head trauma, migraines, or neurological conditions?
- Medication use and recent changes?
Answering these questions helps narrow down potential causes and informs the subsequent physical exam.
Step 2: Physical Examination and Bedside Tests
Neurological Assessment
Doctors evaluate balance, coordination, and reflexes using tests such as:
- Romberg test (standing with feet together, eyes closed)
- Past pointing (patient points to a target with eyes closed)
- Finger‑to‑nose and heel‑to‑shin coordination
Ear, Nose, and Throat (ENT) Examination
A routine otoscopic exam checks for ear canal blockage, inflammation, or fluid. If abnormalities are found, audiological tests may follow.
Step 3: Specialized Vestibular Tests
When the initial assessment suggests vertigo, more precise tests are ordered. These include:
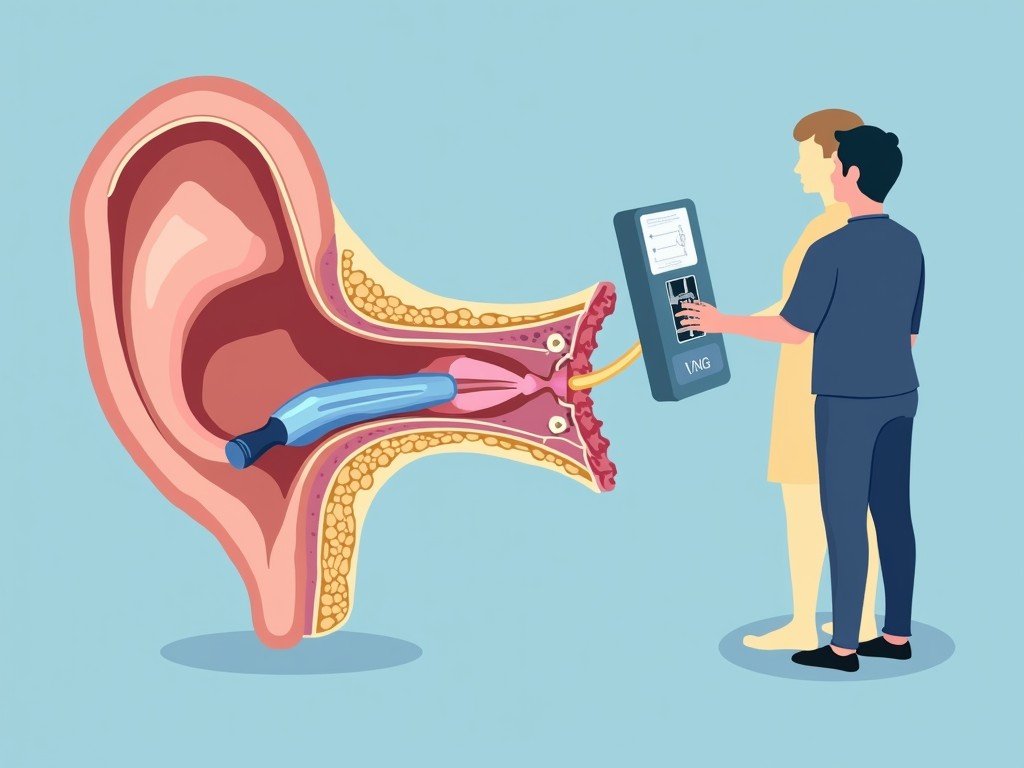
Video Nystagmography (VNG)
VNG records eye movements using infrared cameras while the patient performs a series of gaze and positional tests. It helps differentiate peripheral from central causes by evaluating the vestibulo‑ocular reflex (VOR).
Dix‑Hallpike Maneuver
Essential for diagnosing benign paroxysmal positional vertigo (BPPV). The patient sits, turns the head 45° to one side, then lies back quickly with the head hanging 30° below the horizontal. A characteristic nystagmus indicates BPPV.
Caloric Test
Each ear is irrigated with warm and cold water or air to stimulate the horizontal semicircular canal. The resulting eye movements reveal asymmetry or weakness in vestibular function.
Video Head Impulse Test (V‑HIT)
V‑HIT evaluates the high‑velocity VOR by rapidly turning the head while recording eye movements. It’s particularly useful for detecting deficits in the semicircular canals.
Computerized Dynamic Posturography (CDP)
CDP simulates real‑world balance challenges by varying visual, vestibular, and proprioceptive inputs. It provides a comprehensive view of how the patient maintains equilibrium in different environments.
Interpreting the Results
Each test yields specific data points:
- VNG: Presence of spontaneous nystagmus, gaze‑evoked nystagmus, or positional nystagmus.
- Dix‑Hallpike: Direction and latency of nystagmus, indicating BPPV.
- Caloric: Asymmetry ratio, indicating unilateral vestibular weakness.
- V‑HIT: Gain values below 0.8 suggest canal dysfunction.
- CDP: Scoring on the Sensory Organization Test (SOT) reveals reliance on visual or proprioceptive cues.
When peripheral signs dominate, treatment focuses on canalith repositioning or medication. Central findings prompt imaging (MRI/CT) and referral to a neurologist.
Common FAQs About Vertigo Diagnosis
- Q: How long does a vertigo evaluation take?
A: Initial history and exam can be done in 30–45 minutes; specialized tests may require a separate appointment. - Q: Are these tests painful?
A: Most are non‑invasive; the caloric test may cause mild discomfort. - Q: Can vertigo be diagnosed without imaging?
A: Yes, if peripheral signs are clear, imaging may be unnecessary.
Conclusion: The Path to Relief Starts with Accurate Diagnosis
Vertigo can be a frustrating and debilitating symptom, but a systematic diagnostic approach—starting with a thorough history, followed by targeted physical and vestibular tests—provides the roadmap to effective treatment. Whether the cause is a benign inner‑ear disorder or a more serious central lesion, early and precise diagnosis is key to restoring balance and improving quality of life.
If you’re experiencing vertigo symptoms, consult a qualified ENT or neurologist. With the right diagnostic tools and expertise, you can move from uncertainty to a clear, personalized treatment plan.