Paranasal Sinus Osteoma: Diagnosis, Symptoms, and Endoscopic Treatment Options
Paranasal sinus osteoma is a rare, benign bone tumor that can silently grow within the sinus cavities of the skull. While many patients remain asymptomatic, the potential for nasal obstruction, facial pain, and even visual disturbances makes early recognition and appropriate management essential. This guide provides a comprehensive overview of paranasal sinus osteoma, covering its causes, clinical presentation, diagnostic work‑up, and the latest endoscopic surgical techniques that offer effective, minimally invasive treatment.
What Is a Paranasal Sinus Osteoma?
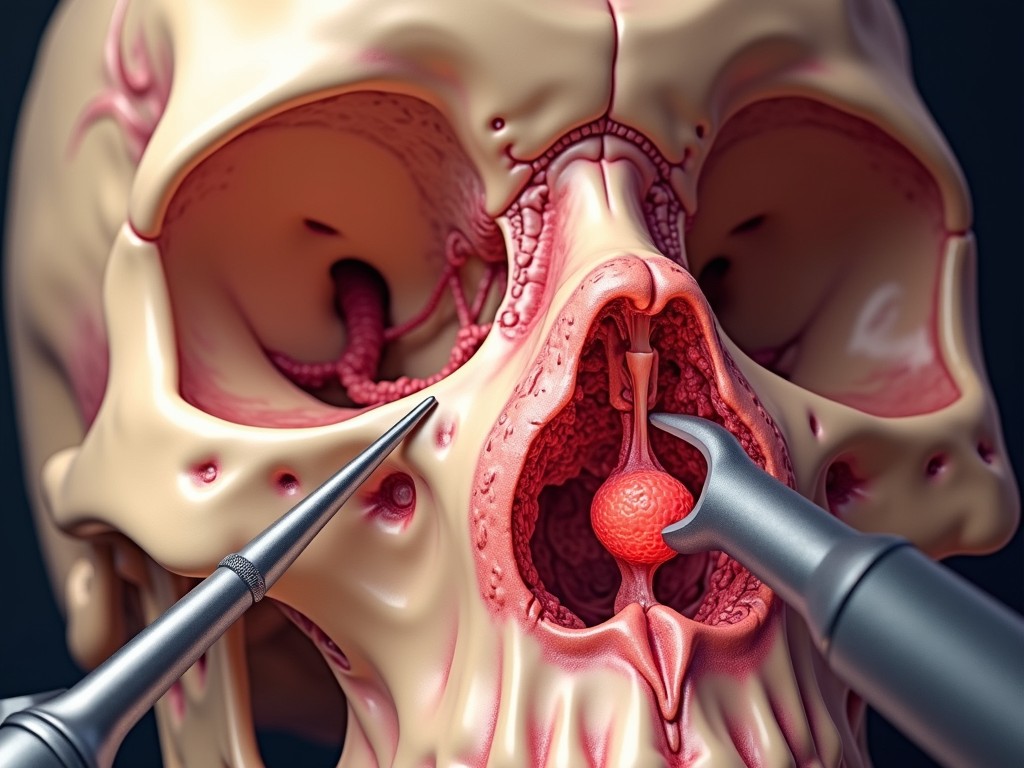
Paranasal sinus osteoma is a slow‑growing, benign bone tumor that originates from the bony walls of the sinus cavities. The most common sites are the frontal sinus (above the brow) and the ethmoid sinus (between the nose and the eyes). Less frequently, osteomas may arise in the maxillary or sphenoid sinuses. Because these lesions are typically asymptomatic, they are often discovered incidentally during imaging studies performed for unrelated reasons.
Causes and Risk Factors
The exact etiology of sinus osteoma remains unclear. However, several factors are thought to contribute to its development:
- Developmental anomalies – congenital variations in sinus bone formation.
- Trauma – repeated blows to the face or skull can trigger abnormal bone growth.
- Chronic infections – long‑standing sinusitis may stimulate bone proliferation.
- Genetic predisposition – family history of bone tumors or craniofacial syndromes.
Clinical Presentation
Most osteomas are asymptomatic and do not require intervention. When they grow large enough to impinge on surrounding structures, patients may experience:
- Persistent nasal congestion or blockage
- Frontal or orbital pain
- Visual disturbances such as blurred vision or double vision
- Facial asymmetry or deformity
- Recurrent sinus infections (sinusitis)
Diagnostic Work‑Up
The gold standard for diagnosing a sinus osteoma is computed tomography (CT). CT imaging reveals a dense, bone‑like lesion that partially or completely fills the sinus cavity. In selected cases, magnetic resonance imaging (MRI) may be employed to assess soft‑tissue involvement or to rule out other pathologies.
When Is Treatment Needed?
Not every osteoma requires surgery. Treatment is typically reserved for:
- Lesions causing significant symptoms (nasal obstruction, pain, visual changes)
- Large or rapidly growing tumors that threaten adjacent structures
- Patients with cosmetic concerns or facial deformity
- Osteomas associated with recurrent sinusitis that is refractory to medical therapy
Endoscopic Sinus Surgery: The Preferred Approach
Endoscopic sinus surgery (ESS) has become the standard of care for most sinus osteomas. This minimally invasive technique offers several advantages:
- No external incisions – no visible scars
- Shorter hospital stay and faster recovery
- Reduced risk of bleeding and infection
- Excellent visualization of the surgical field using high‑definition cameras
Procedure Overview
During ESS, the surgeon inserts a nasal endoscope through the nostril, using specialized micro‑tools to carefully remove the osteoma. The procedure is guided by pre‑operative imaging and, in complex cases, by intra‑operative navigation systems that provide real‑time feedback on the tumor’s location relative to critical structures such as the optic nerve and the brain.
When Is Open Surgery Considered?
Open surgical approaches are reserved for:
- Very large osteomas that cannot be fully accessed endoscopically
- Tumors that have extended beyond the sinus cavity into adjacent bone or soft tissue
- Cases where the osteoma is located near the eye or brain and requires a more controlled approach
Common open techniques include frontal osteotomy, lateral rhinotomy, and bicoronal approaches. These procedures involve external incisions and are typically performed by a multidisciplinary team that may include neurosurgeons or ophthalmologists.
Post‑Operative Care and Follow‑Up
After surgery, patients usually experience:
- Minor nasal congestion that resolves within a few days
- Possible mild swelling or bruising around the eyes or forehead
- Need for nasal saline rinses to keep the surgical site clean
Regular follow‑up appointments are essential to monitor for recurrence, which is rare but possible. Imaging studies (usually CT) are performed at 6 months and then annually if the osteoma was large or symptomatic.
Frequently Asked Questions
- Is a sinus osteoma cancerous? No. Osteomas are benign bone tumors with no malignant potential.
- Can osteomas grow back after removal? Recurrence is uncommon but can occur, especially if the tumor was not completely excised. Close follow‑up helps detect any regrowth early.
- What are the risks of endoscopic surgery? As with any surgery, risks include bleeding, infection, and injury to nearby structures. However, ESS has a low complication rate when performed by experienced surgeons.
- Will I need a permanent nasal cast or splint? Typically, no. The endoscopic approach avoids external incisions, so no external splints are required.
- How long does recovery take? Most patients resume normal activities within 1–2 weeks, though complete healing may take up to 4 weeks.
Conclusion
Paranasal sinus osteoma is a rare, benign bone tumor that can remain silent or cause significant symptoms depending on its size and location. Early detection through imaging, coupled with modern endoscopic surgical techniques, allows for safe, effective treatment with minimal morbidity. If you experience persistent nasal congestion, facial pain, or visual changes, consult an ENT specialist for evaluation. With timely intervention, patients can achieve excellent outcomes and a return to normal life.
For more information or to schedule a consultation, contact Dr. Gediz Murat Serin, a leading otolaryngologist specializing in sinus and skull base surgery.