Hiatal Hernia Explained: Symptoms, Causes, and Effective Treatment Options
Introduction
Have you ever felt a burning sensation in your chest after a meal, or experienced difficulty swallowing that seems to worsen over time? These uncomfortable symptoms could be more than just indigestion—they might signal a hiatal hernia, a condition that affects millions worldwide. Understanding what a hiatal hernia is, recognizing its signs, and exploring both lifestyle and medical treatments can help you regain control over your digestive health.
What Is a Hiatal Hernia?
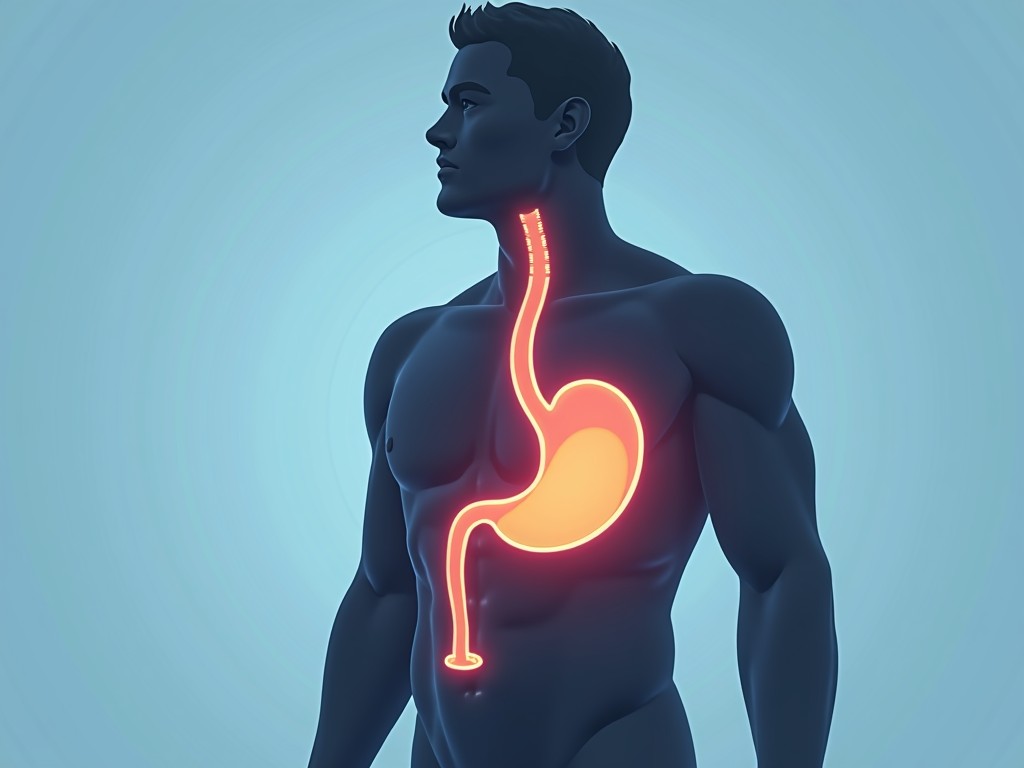
A hiatal hernia, also known as a stomach hernia, occurs when part of the stomach pushes upward through the diaphragm into the chest cavity. The diaphragm normally acts as a barrier, keeping the stomach firmly in the abdominal area. When the muscle or tissue that holds the stomach in place weakens or tears, the stomach can slip through the opening (hiatus) in the diaphragm.
Types of Hiatal Hernias
- Sliding Hiatal Hernia – The most common type, where the junction between the esophagus and stomach slides up into the chest.
- Paraesophageal Hiatal Hernia – A less common but more serious form where part of the stomach herniates beside the esophagus.
- Mixed Hiatal Hernia – A combination of sliding and paraesophageal features.
Common Symptoms to Watch For
Hiatal hernias can be silent, but many people experience a range of uncomfortable symptoms:
- Heartburn and Acid Reflux – Burning sensation in the chest or throat due to stomach acid backing up.
- Chest Pain – Often felt after eating or when lying down.
- Difficulty Swallowing (Dysphagia) – A feeling of food getting stuck.
- Belching and Bloating – Excess gas and a feeling of fullness.
- Regurgitation – Sour or bitter liquid coming back up.
- Shortness of Breath – In severe cases, the hernia can press on the lungs.
Why Does a Hiatal Hernia Occur?
Several factors can weaken the diaphragm or increase abdominal pressure, leading to a hiatal hernia:
- Obesity – Excess abdominal fat puts pressure on the stomach.
- Heavy Lifting – Repeated strain can tear the diaphragm muscle.
- Chronic Cough or Vomiting – Persistent coughing or forceful vomiting raises intra-abdominal pressure.
- Age-Related Muscle Weakness – The diaphragm naturally loses strength over time.
- Smoking – Damages esophageal muscles and promotes acid reflux.
- Genetic Predisposition – Family history can increase risk.
Diagnosing a Hiatal Hernia
Because symptoms overlap with other digestive disorders, a proper diagnosis is essential. Common diagnostic tools include:
- Upper Endoscopy (EGD) – Visual inspection of the esophagus and stomach lining.
- Upper GI Series (Barium Swallow) – X-ray imaging after swallowing a barium solution.
- Esophageal Manometry – Measures pressure and muscle contractions in the esophagus.
- 24‑Hour pH Monitoring – Detects acid reflux episodes.
Treatment Options: From Lifestyle to Surgery
Managing a hiatal hernia often starts with simple lifestyle changes, but more severe cases may require medication or surgery.
1. Lifestyle and Dietary Modifications
- Eat smaller, more frequent meals.
- Avoid trigger foods: spicy, fatty, or acidic items.
- Do not lie down within 3 hours of eating.
- Elevate the head of the bed by 6–8 inches.
- Maintain a healthy weight and engage in regular, gentle exercise.
- Quit smoking and limit alcohol consumption.
2. Medications
- Antacids – Neutralize stomach acid for quick relief.
- H2 Receptor Blockers – Reduce acid production (e.g., ranitidine).
- Proton Pump Inhibitors (PPIs) – Stronger acid suppression (e.g., omeprazole).
- Use under medical supervision to avoid long‑term side effects.
3. Surgical Intervention
When lifestyle changes and medications fail, or if the hernia is large or causing complications, surgery may be recommended. The most common procedure is the Nissen fundoplication, where the upper part of the stomach is wrapped around the lower esophagus to reinforce the valve and prevent reflux. Modern laparoscopic techniques allow for minimally invasive surgery with shorter recovery times.
Frequently Asked Questions
Is a hiatal hernia dangerous?
Most hiatal hernias are benign, but complications such as strangulation, bleeding, or severe reflux can occur. Prompt treatment can mitigate risks.
Can I prevent a hiatal hernia?
While genetics play a role, maintaining a healthy weight, avoiding heavy lifting, and quitting smoking can reduce the likelihood of developing a hernia.
Will surgery cure the symptoms?
In many cases, surgery resolves reflux and pain. However, some patients may still experience mild symptoms post‑operatively, especially if lifestyle changes are not sustained.
Conclusion
A hiatal hernia can be a source of persistent discomfort, but with a clear understanding of its causes, symptoms, and treatment options, you can take proactive steps toward relief. Start with simple dietary and lifestyle adjustments, consult your healthcare provider for proper diagnosis, and consider medication or surgery if needed. By combining medical care with healthy habits, you can manage or even eliminate the impact of a hiatal hernia on your daily life.